👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Sleep and Heart Disease: What Every Patient Needs to Know
The connection between sleep and heart disease is one of the most clinically important and least discussed relationships in cardiovascular medicine. Poor sleep quality, particularly from untreated sleep-disordered breathing, directly strains the cardiovascular system overnight.
This article reflects the clinical expertise of Dr. Avinesh Bhar, Board Certified Sleep Physician at Sliiip.com. He evaluates the sleep-heart connection in patients who have often been treated for years for heart issues without anyone addressing what is happening to their breathing during sleep.
Sleep and heart disease are not parallel concerns. They are part of the same physiological story, and the overnight hours are where a critical chapter goes unread.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
Myth vs. Reality: Sleep and Heart Disease
Myth: Heart disease is primarily a daytime problem driven by diet, exercise, and stress. Sleep is a secondary concern.
Reality: The overnight hours are when the cardiovascular system performs essential recovery and when, in people with untreated sleep apnea, it experiences repeated physiological assault through oxygen deprivation and stress hormone surges. Sleep is not a passive rest state for the heart. It is an active period of cardiovascular regulation.
Myth: If your sleep apnea is not severe, it probably does not significantly affect your heart.
Reality: Even mild to moderate sleep apnea generates repeated overnight oxygen desaturations and sympathetic nervous system activations that elevate blood pressure and increase cardiac workload night after night.
How Sleep Regulates the Cardiovascular System
During healthy sleep, the cardiovascular system undergoes organized changes that are essential for long-term cardiac health. Blood pressure drops by ten to twenty percent during the night in a process called nocturnal dipping. Heart rate slows. The sympathetic nervous system, which drives the fight-or-flight response and elevates cardiac demand, becomes less active. Parasympathetic activity, which promotes recovery and cardiac repair, predominates.
Sleep-disordered breathing is the leading cause of non-dipping patterns in otherwise healthy adults.
Sleep apnea symptoms include loud snoring, gasping during sleep, morning headaches, dry mouth, and significant daytime fatigue. These symptoms emerge from repeated partial or complete airway collapse during sleep, which fragments rest and reduces oxygen delivery to the brain and body.
Sleep Apnea: The Primary Mechanism Connecting Sleep and Heart Disease
Obstructive sleep apnea is the most clinically important intersection of sleep and heart disease. Every apnea event initiates a cascade of cardiovascular stressors.
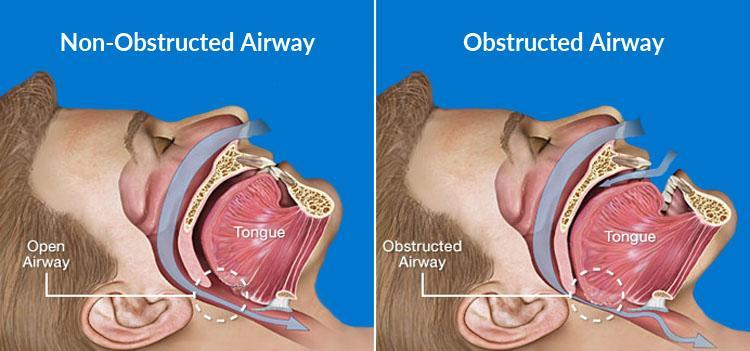
When the airway collapses and breathing pauses, blood oxygen levels fall. The brain detects the oxygen drop and activates the sympathetic nervous system to restore breathing. This activation surges adrenaline and cortisol, spikes heart rate, and elevates blood pressure. The effect is comparable to a brief physiological alarm response, repeated dozens to hundreds of times per night.
Over months and years, these repeated overnight surges produce durable structural and functional cardiovascular damage. Blood vessel walls thicken. Arterial stiffness increases.
Dr. Avinesh Bhar regularly sees patients whose blood pressure control has been notoriously difficult for years, who have been on multiple antihypertensive agents, and whose clinical picture transforms after a home sleep evaluation reveals moderate or severe sleep apnea.
For patients undergoing atrial fibrillation treatment, sleep apnea evaluation is not optional. It is part of the clinical picture. Learn more about recognized sleep apnea symptoms.
Sleep, Heart Disease Risk, and Heart Failure
The connection between sleep and heart disease extends directly to heart failure. Sleep apnea is present in up to 50 percent of heart failure patients, though it is formally diagnosed in a significantly smaller proportion.
The relationship is bidirectional. Sleep apnea worsens heart failure through chronic nocturnal pressure overload and sympathetic activation. Heart failure can trigger or worsen sleep apnea by causing fluid redistribution to the upper airway during recumbent sleep.
What is Sleep Apnea?
In patients with existing heart failure, identifying and addressing sleep-disordered breathing is one of the most impactful clinical steps for stabilizing the condition and improving functional outcomes. Sleep and heart disease management must be integrated to be effective.
Women, Sleep, and Heart Disease
The sleep-heart disease relationship has particular significance for women, who are consistently underdiagnosed with sleep apnea and who face distinct cardiovascular consequences when it goes untreated.
Research documents that women with undetected sleep apnea have a disproportionately elevated risk of heart disease compared to men with the same apnea severity. This disparity is partly attributed to the longer diagnostic delay women experience.
A home sleep test is the easiest way to test for sleep apnea. Sliiip.com ships the testing device directly to your home. You wear it overnight in your own bed. A board-certified sleep physician reviews the results and can identify whether breathing disruptions are fragmenting your sleep architecture.

Learn more about how the home sleep test works.
You do not need a referral. You do not need to fit a snoring stereotype. You need an honest look at what is happening during those eight hours.
Our home sleep tests are covered by Medicare, Tricare and these insurances listed below.

Expert Q&A
Q: I am a 54-year-old woman. I have been on three blood pressure medications for two years. My cardiologist says my pressure is still not fully controlled, especially in the mornings. No one has mentioned sleep. Should they have?
Yes, they should have. Resistant hypertension, defined as blood pressure that remains elevated despite multiple medications, is one of the strongest clinical indications for sleep apnea evaluation in the literature. Morning hypertension specifically, where readings are highest upon waking, is a recognized pattern of nocturnal sympathetic activation from apnea events. The cardiovascular system does not reset properly overnight when breathing is disrupted repeatedly. If you have never had an overnight breathing evaluation and your blood pressure is difficult to control, that evaluation should happen before the next medication adjustment.
Dr. Avinesh Bhar Board Certified Sleep Physician Sliiip.com
Practical Steps at the Intersection of Sleep and Heart Disease
Consistent sleep timing supports heart rate variability. Heart rate variability, a marker of cardiac autonomic health, is significantly influenced by sleep regularity. Going to bed and waking at the same time every day improves the overnight parasympathetic recovery that benefits cardiac function.
Limit alcohol, particularly in the evening. Alcohol fragments sleep architecture, suppresses parasympathetic activity during sleep, and increases nocturnal blood pressure variability. Its acute cardiovascular effects during sleep are opposite to the restorative cardiovascular changes that healthy sleep promotes.
Side sleeping reduces apnea events. Supine sleeping worsens airway collapse and increases apnea frequency. Side sleeping reduces the gravitational obstruction component and is associated with lower apnea-hypopnea index scores in many people. This simple positional change is the lowest-barrier intervention for people with known or suspected sleep apnea.
Address nasal obstruction. Anything that increases upper airway resistance during sleep increases the cardiovascular load associated with each breath. Managing chronic nasal congestion through allergy treatment, saline rinse, or anatomical correction reduces breathing effort and the associated sympathetic activation.
Could undetected sleep apnea be undermining your cardiovascular health every night?
Sliiip.com has completed over 10,000 consultations with patients across all 50 states. No referral is needed. Home sleep testing ships directly to your door and is covered by most major insurance plans including Medicare and Tricare.
Frequently Asked Questions
How does poor sleep affect heart disease risk?
Poor sleep, particularly from sleep apnea, increases heart disease risk through repeated overnight oxygen drops, elevated blood pressure, sustained sympathetic nervous system activation, chronic inflammation, and disrupted nocturnal cardiovascular recovery. These mechanisms produce cumulative cardiac strain that increases risk for hypertension, atrial fibrillation, coronary artery disease, and stroke.
Does sleep apnea cause heart disease?
Research from the American Heart Association supports a strong association between untreated obstructive sleep apnea and multiple forms of heart disease, including hypertension, atrial fibrillation, coronary artery disease, heart failure, and stroke. Sleep apnea is now recognized as an independent cardiovascular risk factor requiring clinical attention.
Can fixing sleep apnea improve heart health?
Evidence suggests that effective sleep apnea treatment reduces nocturnal blood pressure, improves heart rate variability, and lowers some inflammatory markers associated with cardiovascular disease. While treatment is most impactful when initiated before structural damage is established, improvements in cardiac stress parameters have been observed even in patients with existing cardiovascular conditions.
What is the relationship between sleep apnea and high blood pressure?
Sleep apnea is the leading identifiable cause of secondary hypertension. Overnight sympathetic surges from apnea events chronically elevate blood pressure and prevent the nocturnal dipping that allows the cardiovascular system to recover. Patients with blood pressure that is difficult to control on multiple medications have a high prevalence of undetected sleep apnea.
Can sleep deprivation cause a heart attack?
Research shows that chronically short sleep duration is associated with elevated cardiovascular event risk. The mechanisms include elevated cortisol, increased inflammatory markers, reduced glucose regulation, and impaired endothelial function. Sleep deprivation is a modifiable cardiovascular risk factor comparable in significance to smoking and sedentary behavior.
Is atrial fibrillation linked to sleep apnea?
Yes. Sleep apnea is significantly associated with atrial fibrillation onset and recurrence after treatment. Nocturnal oxygen drops and sympathetic activation alter atrial electrical properties and promote atrial enlargement, both of which increase arrhythmia susceptibility. Treating sleep apnea is an important component of atrial fibrillation management.
What is nocturnal blood pressure and why does it matter?
Nocturnal blood pressure refers to blood pressure levels during sleep. In healthy individuals, blood pressure drops ten to twenty percent overnight, a pattern called dipping, which allows cardiovascular recovery. Sleep apnea prevents this dip, maintaining elevated nighttime pressure. Non-dipping is associated with significantly elevated risk of cardiac events independent of daytime blood pressure.
How does sleep affect the heart at night?
During healthy sleep, heart rate slows, blood pressure drops, sympathetic activity decreases, and parasympathetic recovery predominates. These changes allow cardiac muscle recovery, vessel wall repair, and autonomic rebalancing. In sleep apnea, each breathing event reverses these protective changes through sympathetic activation, elevated pressure, and oxygen deprivation.
Can heart disease cause sleep problems?
Yes. Heart failure, in particular, can cause central sleep apnea and Cheyne-Stokes breathing, patterns of disordered breathing that disrupt sleep quality. Cardiac medications including diuretics may cause nocturia. Chest discomfort and orthopnea can disrupt sleep onset and maintenance. The relationship between sleep and heart disease is bidirectional.
Should heart patients get a sleep study?
Yes. Major cardiology organizations now recommend sleep apnea evaluation as part of comprehensive cardiovascular risk management, particularly for patients with resistant hypertension, atrial fibrillation, heart failure, or unexplained daytime fatigue. A home sleep test is a comfortable, accessible entry point that does not require a clinic overnight stay.
Does poor sleep raise cholesterol?
Research links chronic sleep restriction and fragmentation to elevated LDL cholesterol, reduced HDL cholesterol, and worsened triglyceride profiles. Sleep deprivation disrupts lipid metabolism and promotes the inflammatory environment that accelerates atherosclerotic plaque development. Optimizing sleep quality is a legitimate metabolic intervention alongside dietary and pharmacological approaches.
Can improving sleep lower blood pressure?
Yes. Effective treatment of sleep apnea has been shown to reduce daytime and nocturnal blood pressure in hypertensive patients. Even without sleep apnea, improvements in sleep duration and quality are associated with modest but measurable reductions in blood pressure through cortisol and sympathetic activity normalization.
Latest posts
-
Is My Sleep Pattern Normal? What a Normal Sleep Pattern Looks Like
If you have ever lain awake wondering whether your nights match everyone else’s, learning what a normal sleep pattern looks like can bring real peace of mind, says Dr. Avinesh…
-
Spike in Cortisol: How Workplace Stress Destroys Men’s Sleep Cycles
After a long, high pressure day at work, a spike in cortisol can follow men straight into the bedroom and quietly wreck a good night of rest, says Dr. Avinesh…
-
Overthinking at Night
Overthinking at night can turn the quietest hours into the loudest part of the day, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, hears this complaint more than almost…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

