👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Can CPAP Cause Headaches? What to Do Now?
You started CPAP therapy to feel better, not worse. So when you wake up with a pounding headache after using your machine, it is understandable to wonder can CPAP cause headaches?
Quick Answer: Yes, CPAP therapy can cause headaches, but they are usually fixable. Common causes include mask pressure that is too high, air swallowing (aerophagia), sinus congestion from inadequate humidification, and mask fit issues. Research shows 54.3% of sleep apnea patients report morning headaches, but CPAP therapy actually improves headaches in 81.3% of cases when properly adjusted.
“Headaches are one of the most common complaints I hear from new CPAP users,” says Dr. Avinesh Bhar, founder of SLIIIP and board-certified sleep medicine physician. “But here is what most patients do not realize: the headaches usually mean something specific is wrong with their setup. Fix the root cause, and the headaches disappear. The worst thing you can do is stop therapy altogether.”
Struggling with CPAP headaches? SLIIIP’s sleep specialists can review your therapy data and help optimize your settings for better results and fewer side effects.
Important: Sleep Apnea Headaches vs. CPAP Headaches
Before blaming your CPAP machine, understand that untreated sleep apnea itself causes morning headaches. According to the International Classification of Headache Disorders (ICHD-3), sleep apnea headaches typically occur upon waking, last less than 4 hours, and resolve with effective treatment.
Research shows that 54.3% of sleep apnea patients experience morning headaches before treatment. When CPAP therapy is properly prescribed and used correctly, 81.3% of those patients see improvement in their headaches.
Key distinction: If you had morning headaches before starting CPAP, your machine may be undertreating your sleep apnea. If headaches only started after beginning CPAP therapy, something about your setup likely needs adjustment.
6 Reasons Your CPAP May Be Causing Headaches
- Pressure is Set Too High
When CPAP pressure exceeds what your body needs, you may unconsciously fight the airflow during sleep. This creates tension in your jaw, neck, and facial muscles, leading to tension-type headaches. If your headaches feel like a band squeezing around your head, excessive pressure may be the culprit.
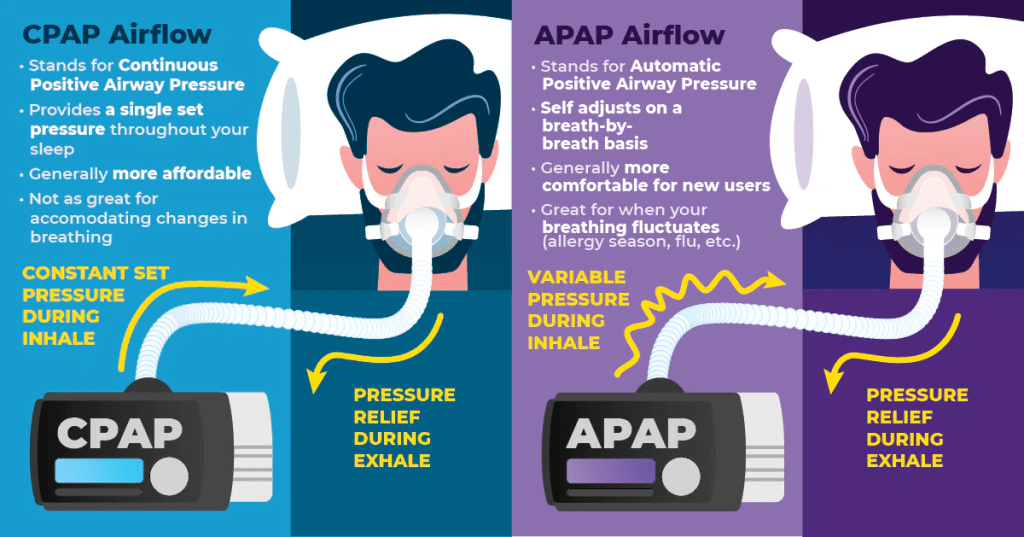
Solution: Request a pressure adjustment from your sleep specialist. Many patients benefit from switching to APAP (auto-adjusting) therapy, which automatically finds the minimum pressure needed throughout the night.
- Air Swallowing (Aerophagia)
Swallowing air during CPAP use causes bloating, stomach discomfort, and sometimes headaches. This happens when pressure is too high, when you breathe through your mouth with a nasal mask, or when the mask seal is poor and you gulp air to compensate.
Solution: Try lowering pressure, switching to a full face mask, or using a chin strap to keep your mouth closed. Sleeping with your head slightly elevated can also help.
- Sinus Congestion and Dry Air
CPAP delivers a constant stream of air that can dry out your nasal passages and sinuses, especially in dry climates or during winter months. This leads to sinus pressure, congestion, and frontal headaches.
Solution: Use a heated humidifier with your CPAP machine. Start at a low humidity setting and increase gradually until symptoms improve. Some patients also benefit from saline nasal spray before bed.
- Mask Fit Problems
A mask that is too tight creates pressure points on your face, forehead, and temples. Over 6 to 8 hours of sleep, this constant pressure causes headaches. A mask that is too loose causes air leaks that disrupt sleep quality and may lead to undertreated apnea.
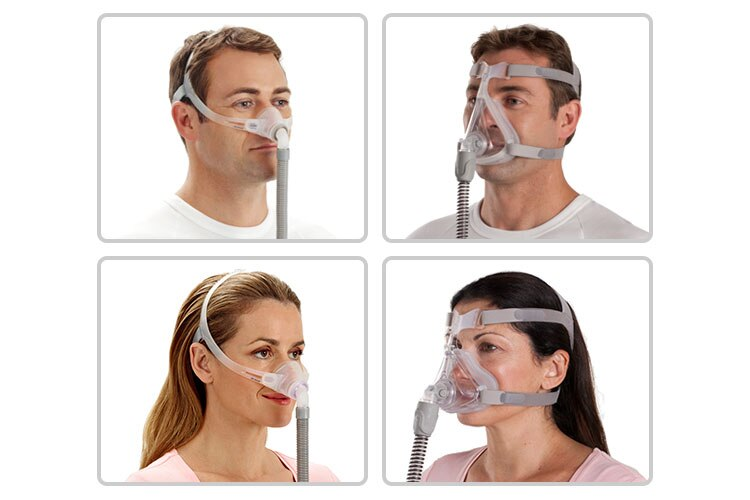
Solution: Get a professional mask fitting with a sleep specialist. The mask should seal without being cranked down tight. Consider trying a different mask style (nasal pillows, nasal mask, or full face mask) to find the best fit for your face shape.
- Carbon Dioxide Rebreathing
Some mask designs can trap exhaled carbon dioxide if the exhalation port is blocked or if you are using incompatible equipment. Rebreathing CO2 causes morning headaches, grogginess, and poor sleep quality.
Solution: Check that your mask’s exhalation ports are clear and unobstructed. Never use a mask designed for one machine type with a different type of CPAP or BiPAP.
- Undertreated Sleep Apnea
If your CPAP settings are not adequate for your sleep apnea severity, you may still experience apnea events and oxygen desaturation during sleep. This causes the same morning headaches you had before treatment.
Solution: Review your CPAP data with your sleep specialist. If your AHI is still elevated while using the machine, your settings need adjustment. You may need a new sleep study to reassess your condition.
When to See a Doctor About CPAP Headaches
Most CPAP headaches resolve with simple adjustments. However, contact your sleep specialist if:
Headaches persist despite troubleshooting
You experience severe headaches that wake you from sleep
Headaches are accompanied by confusion, vision changes, or neurological symptoms
You have stopped using your CPAP because of headaches
“Never stop CPAP therapy on your own because of headaches,” emphasizes Dr. Bhar. “Untreated sleep apnea puts you at serious risk for stroke, heart attack, and other complications. Work with your sleep team to solve the headache problem while keeping your therapy going.”
Frequently Asked Questions
Q: How long do CPAP headaches last?
A: CPAP-related headaches typically resolve within a few hours of waking. If headaches last all day, they may be caused by something other than your CPAP therapy.
Q: Can a dirty CPAP machine cause headaches?
A: Yes. Mold, bacteria, and mineral buildup in your humidifier or tubing can cause sinus irritation and headaches. Clean your equipment regularly following manufacturer guidelines.
Q: Will switching to BiPAP help with CPAP headaches?
A: Possibly. BiPAP uses different pressure levels for inhaling and exhaling, which can reduce air swallowing and discomfort for some patients. Talk to your sleep specialist about whether BiPAP might be appropriate for you.
Q: Should I take pain medication before using my CPAP?
A: Taking pain medication to preemptively treat CPAP headaches is not recommended. It is better to identify and fix the root cause. If you need pain relief, over-the-counter options like acetaminophen or ibuprofen are generally safe, but consult your doctor.
The Bottom Line
CPAP therapy can cause headaches, but this is almost always a solvable problem. Check your pressure settings, mask fit, and humidification levels before considering major changes. Most importantly, do not abandon your therapy because of headaches. The consequences of untreated sleep apnea are far more serious than the temporary discomfort of adjusting to CPAP treatment.
Need Help Optimizing Your CPAP Therapy? SLIIIP’s board-certified sleep medicine physicians can review your CPAP data remotely and help you troubleshoot headaches and other side effects. Our telemedicine approach means you get expert guidance without leaving home. Schedule your consultation at sliiip.com or call 478-238-3552
Latest posts
-
Digital Insomnia Therapy: A Doctor’s Guide to the Drug-Free Fix for Sleepless Nights
Digital insomnia therapy has quietly become one of the most effective tools in modern sleep medicine, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and many people now use…
-
AI Powered Apps for Sleep: A Doctor’s Guide to the Best Tools on Your Phone
AI powered apps for sleep now sit on more than half a billion phones around the world, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and patients walk into…
-
AI for Sleep: How Artificial Intelligence Is Changing the Way We Rest
AI for sleep has become a quiet revolution in how people fall asleep, stay asleep, and figure out what is wrong with their nights, says Dr. Avinesh Bhar, Board-Certified Sleep…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

