👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET
Do I Need a Sleep Study?
You have been dragging through your days for months. The fatigue is relentless. You wake up feeling like you barely slept, and you wonder “do I need a sleep study?”
At some point, the question forms: should I actually get tested? Is what I am experiencing normal, or is it a sign that something deserves a closer look?
If you are asking yourself whether you need a sleep study, that question alone is worth taking seriously. Dr. Avinesh Bhar works with home sleep tests that are delivered right to your home. They are often covered by insurance and can accurately diagnose issues like sleep apnea.
What a Sleep Study Actually Tells You
A sleep study is a monitoring process that records what happens in your body while you rest. It captures data on breathing patterns, oxygen levels, heart rate, brain activity, and body movement, painting a detailed picture of your sleep quality that you simply cannot observe on your own.
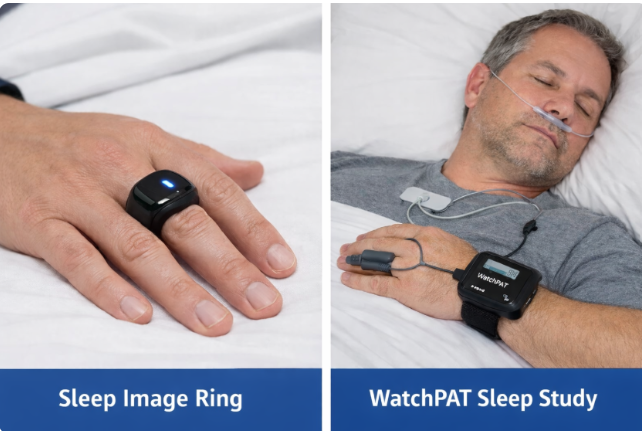
At SLIIIP we use home sleep testing devices (HST) such as Sleep Image Ring and the WatchPat.
These devices are covered by Medicare, Tricare and these major insurances shown below.

The most common reason people are recommended for a sleep study is to evaluate breathing-related disruptions during the night. These disruptions, which can occur dozens or even hundreds of times per night, often happen without fully waking you. You may have no idea they are occurring, but their impact on your daytime energy, mood, and cognitive function can be significant.
Sleep studies can be conducted in a clinical lab or, increasingly, in the comfort of your own home. A home sleep test uses a small, portable device that monitors your breathing, oxygen saturation, and other key metrics while you rest in your own bed. It is a simpler, more accessible option that works well for evaluating breathing-related concerns.
Signs That Point Toward Testing
Not every rough night warrants a sleep study. But certain patterns, especially when they persist over weeks or months, suggest that your rest quality may be compromised by something beyond lifestyle factors.

Consider whether you experience any of the following on a regular basis. Loud or disruptive snoring that your partner or household members have noticed. Waking up gasping, choking, or feeling short of breath during the night. Persistent morning headaches or a dry mouth upon waking. Excessive daytime fatigue despite spending adequate time in bed. Difficulty concentrating, brain fog, or memory problems. Frequent nighttime awakenings without a clear cause. Falling asleep unintentionally during the day, such as while watching television, reading, or even driving.
If several of these resonate, a sleep evaluation is a practical and worthwhile step. You do not need to have every symptom on the list. Even two or three persistent patterns may indicate that your rest is being disrupted in ways that affect your health and quality of life.
Why Get Tested?
Some people hesitate because they wonder if their symptoms are “bad enough” to justify testing. This is a common and understandable concern. However, sleep apnea is far more prevalent than most people realize, and many individuals live with it for years without a diagnosis. Sleep studies are not reserved for extreme cases. They are diagnostic tools designed to provide clarity, even when symptoms seem mild or inconsistent.
Obstructive sleep apnea affects millions of adults and often goes undetected, particularly when symptoms are subtle or attributed to stress, aging, or a busy lifestyle. If your sleep is affecting your daytime energy, focus, mood, relationships, or overall health, that impact alone is reason enough to seek answers.
As Martin N. Gorman, DDS explains, “Many people with sleep apnea don’t realize they have it, but if you wake tired, snore loudly, or feel restless during the day, these can be signs that your brain and body aren’t getting the rest they need.”
Who Benefits Most from a Sleep Study?
While anyone experiencing persistent rest concerns can benefit from testing, certain factors increase the likelihood that a sleep study will reveal actionable findings.
Anyone experiencing persistent sleep concerns may benefit from testing, especially when symptoms continue over time.
- Excess weight, particularly around the neck and throat, increases the risk of airway narrowing during sleep.
- Men are statistically more likely to experience breathing disruptions, though the condition is common and often underdiagnosed in women as well.
- Advancing age is a factor, as throat muscle tone naturally decreases over time, increasing the likelihood of airway collapse during rest.
- A family history of sleep-related breathing disruptions raises your risk.
- Lifestyle factors such as alcohol use, smoking, and sedating medications can relax the airway and contribute to disrupted breathing.
- Quality sleep affects overall health and wellbeing, making it a practical investment to understand what’s happening during your rest.
The Difference Between Home Testing and Lab Studies
Traditional sleep studies take place in a clinical sleep lab, where a technician monitors you overnight using a comprehensive array of sensors. This approach captures the most detailed data, including brain wave activity, eye movement, and muscle tone, making it the gold standard for complex evaluations.

Home sleep tests are a more streamlined alternative designed specifically to evaluate breathing patterns during rest. They typically monitor airflow, blood oxygen levels, breathing effort, and body position. While they do not capture brain wave data, they are highly effective for identifying the breathing disruptions that are the most common cause of unrefreshing sleep.
For most people whose primary concern is daytime fatigue, snoring, or suspected breathing disruptions, a home sleep test is an excellent starting point. It is more convenient, more comfortable, and can be completed without the unfamiliar environment of a lab. Understanding how to get a home sleep test and what the process involves can help you take this step with confidence.
What Happens After the Test?
Once your sleep data is collected, it is reviewed by a qualified sleep specialist who interprets the results and provides recommendations based on your specific findings. If breathing disruptions are identified, the specialist will discuss the severity and explore options for improving your rest quality.
Many people find the results illuminating. Discovering that your breathing was disrupted 30 or 40 times per hour, without your awareness, can be a powerful motivator for making changes. And the good news is that effective solutions exist. From positional adjustments and lifestyle changes to devices like CPAP equipment and oral appliances, there are options to fit different needs and preferences.
Frequently Asked Questions
What is a sleep study?
A sleep study is a monitoring process that records body functions during sleep, including breathing patterns, oxygen levels, heart rate, and movement, to identify disruptions that may affect rest quality.
How do I know if I need a sleep study?
If you regularly experience loud snoring, daytime fatigue despite adequate time in bed, morning headaches, waking up gasping, or persistent brain fog, a sleep evaluation is worth considering.
Can I take a sleep test at home?
Yes. Home sleep tests use portable devices to monitor breathing and oxygen levels while you rest in your own bed. They are a convenient and effective option for evaluating breathing-related concerns.
Is a home sleep test as accurate as a lab study?
For detecting breathing disruptions, home sleep tests are highly effective. Lab studies capture more detailed data, including brain wave activity, and are recommended for more complex evaluations.
Do I need a doctor’s referral for a sleep study?
In many cases, a referral or prescription is needed. SLIIIP’s telemedicine service can connect you with a qualified professional who can evaluate your symptoms and order the appropriate test.
What does a home sleep test measure?
A home sleep test typically measures airflow, blood oxygen saturation, breathing effort, heart rate, and body position during sleep.
How long does a sleep study take?
A home sleep test is completed during a single night of sleep in your own bed. Lab-based studies also typically require one overnight stay.
Will I be able to sleep during the test?
Most people sleep well enough for the test to gather useful data. Home tests are particularly comfortable because you rest in your familiar environment.
What happens after I get my results?
A sleep specialist reviews your data and discusses findings with you. If disruptions are identified, they will recommend appropriate next steps based on severity and your individual needs.
Is a sleep study covered by insurance?
Many insurance plans cover sleep studies, especially when ordered by a physician based on documented symptoms. Coverage varies by provider and plan.
Can a sleep study detect conditions other than breathing problems?
Lab-based sleep studies can evaluate a range of concerns, including limb movement patterns and sleep stage abnormalities. Home tests are primarily designed to evaluate breathing.
What if my sleep study results are normal?
A normal result is valuable information. It rules out certain conditions and helps direct attention toward other potential causes of your symptoms, such as lifestyle factors or circadian rhythm issues.
Is a sleep study painful or uncomfortable?
No. Sleep studies are non-invasive. Home tests involve wearing a small device with sensors. Lab studies use surface sensors attached with gentle adhesive.
Can I take my regular medications before a sleep study?
In most cases, yes. However, your provider may ask you to avoid certain sleep aids or sedatives beforehand. Always follow the specific instructions given to you.
How soon will I get my results?
Results are typically available within one to two weeks after the study, depending on the provider and the complexity of the data.
Can younger adults need a sleep study?
Yes. Breathing disruptions during sleep affect people of all ages. Younger adults who experience persistent fatigue, snoring, or cognitive fog should not dismiss the possibility of a sleep-related concern.
Does weight affect whether I need a sleep study?
Carrying extra weight, especially around the neck and throat, increases the risk of airway narrowing during sleep. However, breathing disruptions can occur in people of any body type.
Can I just use a fitness tracker to monitor my sleep?
Consumer fitness trackers provide general estimates of sleep duration and stages, but they do not measure breathing patterns or oxygen levels with the accuracy needed to identify clinically significant disruptions.
What should I do to prepare for a home sleep test?
Avoid caffeine and alcohol on the day of the test. Follow your normal bedtime routine. The device comes with instructions for proper sensor placement.
When is the right time to get tested?
If persistent symptoms are affecting your energy, mood, or daily functioning, there is no reason to wait. Earlier testing allows for earlier intervention, which often means simpler and more effective solutions.
Latest posts
-
Why is my sleep getting worse as I get older?
A serious sleep problem is often overlooked. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
How to Know If You Have a Serious Sleep Problem or a Temporary One
A serious sleep problem is often overlooked, according to Dr. Avinesh Bhar Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
Why Do I Wake Up Feeling Worse Than When I Went to Bed? What Waking Up Tired Is Really Telling You
Waking up tired is one of the most common complaints patients bring into the exam room, and it is also one of the most misunderstood, says Dr. Avinesh Bhar, Board-Certified…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

