👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

How to Get a Home Sleep Test: A Step-by-Step Guide
Something keeps waking you up at night, and you are not sure what it is.
Your partner mentions snoring. You wake up with headaches.
Afternoons feel like swimming through fog, no matter how much coffee you drink.
You are wondering how to get a home sleep test because you know there is something wrong. Dr. Avinesh Bhar, CEO of SLIIIP and someone who also suffers from sleep apnea, shares his thoughts on how to do a home sleep test. He and his team of board-certified sleep doctors have helped over 10,000 patients in 40 states sleep better.
Diagnosing sleep apnea traditionally meant spending a night in a sleep laboratory, wired to dozens of sensors while technicians watched you try to sleep in an unfamiliar bed.
Home sleep testing has changed this reality. Today, you can complete a clinically validated sleep study in your own bed, using a device that looks like a large wedding ring, and have results interpreted by a board-certified sleep physician within days.
Here is an example of the Sleep Image ring that is used by SLIIIP and is accepted by health insurance for the home sleep test.
You would sleep with this ring for 2-3 nights and your results will be reviewed by a sleep doctor.

The process is straightforward, the technology is accurate, and the pathway to treatment has never been more accessible.
This guide walks you through every step of getting a home sleep test, from understanding whether you are a candidate to interpreting your results and beginning treatment.
If you feel you may have an issue with sleep apnea and want a home sleep test. SLIIIP has a team of sleep doctors that can assist you.
We accept Medicare, Tricare and most major insurances.

What is a Home Sleep Test?
A home sleep test, also called a home sleep apnea test (HSAT), is an FDA-cleared diagnostic study that monitors your breathing patterns, oxygen levels, and heart rate while you sleep in your own bed. Unlike laboratory polysomnography, which records brain waves, eye movements, and dozens of other physiological signals, home sleep tests focus specifically on detecting sleep-disordered breathing.

Modern home sleep devices use advanced sensors to measure multiple parameters simultaneously. Depending on the device, these may include peripheral arterial tone (changes in blood vessel constriction), pulse oximetry (blood oxygen saturation), heart rate and heart rate variability, respiratory effort, airflow, body position, snoring intensity, and actigraphy (movement patterns that indicate sleep versus wakefulness).
The data collected during your test night is analyzed using sophisticated algorithms that calculate your Apnea-Hypopnea Index (AHI), the number of times per hour your breathing stops (apnea) or becomes significantly shallow (hypopnea). An AHI of less than 5 is considered normal. An AHI of 5 to 14 indicates mild sleep apnea, 15 to 29 indicates moderate sleep apnea, and 30 or higher indicates severe sleep apnea.
Home sleep tests are specifically designed to diagnose obstructive sleep apnea (OSA), which accounts for approximately 90% of all sleep apnea cases. OSA occurs when the muscles in your throat relax during sleep and temporarily block your airway. The test can also detect central sleep apnea in some cases, though complex sleep disorders typically require in-laboratory testing.
SLIIIP.COM connects you with board-certified sleep medicine physicians for personalized treatment plans delivered through convenient telemedicine. Whether you’re struggling with sleep apnea, need a home sleep test or want to address ongoing sleep issues, our doctors provide expert care from the comfort of your home. Call 478-238-3552 to schedule your consultation.
You can also book online and we will contact you within 24 hours for an appointment. Trusted by over 10,000 patients, you are in good hands with SLIIIP
We accept these Medicare, Tricare and these major insurances.

Who is a Good Candidate for Home Sleep Testing?
✅ Good candidate for home sleep testing if:
☐ Loud, chronic snoring
☐ Pauses in breathing during sleep (witnessed)
☐ Gasping or choking at night
☐ Excessive daytime sleepiness
☐ Morning headaches or dry mouth
✅ Higher risk for obstructive sleep apnea if:
☐ BMI ≥ 30
☐ Large neck (Men >17”, Women >16”)
☐ Middle-aged or older
☐ Recessed chin or enlarged tonsils
🚫 Home testing is NOT for diagnosing:
☐ Narcolepsy
☐ Restless leg syndrome
☐ Periodic limb movement disorder
☐ Parasomnias (e.g., sleepwalking)
Step-by-Step Process
- Book your meeting with a sleep doctor
Have a brief visit (30 minutes) with a licensed clinician via zoom to discuss your sleep issues and the next steps.
Book My Sleep Doctor - Receive your test kit
The device is mailed to your home or picked up locally.
Includes instructions and sensors (finger probe, wrist unit, or chest sensor).
4. Do the test at home (3 nights)
Follow your normal routine.
Attach the sensors, turn on the device, and sleep as usual.

- Return or discard the device
• Disposable test → throw away after use
• Reusable test → mail back with prepaid label or drop off - Get your results
A board-certified sleep physician reviews your data.
Results are usually ready in 1–7 business days, followed by a discussion of next steps and treatment options.
Popular Home Sleep Test Devices
Several FDA-cleared home sleep test devices are commonly available, each with different features and capabilities.
Your sleep doctor from SLIIIP will choose one of these devices based on your insurance coverage.
- The SleepImage Ring is a small, comfortable ring worn on your finger that helps your doctor understand how you sleep at home over several nights. While you sleep, it gently tracks your heart rate, oxygen levels, and breathing patterns using a light-based sensor. Collecting data over multiple nights allows the ring to capture changes in your sleep that may not appear in just one night. The SleepImage Ring provides helpful insights into sleep quality and breathing stability, supporting the evaluation of sleep concerns such as sleep apnea and insomnia. Its reusable, easy-to-wear design makes it a convenient and stress-free option for at-home sleep testing.
- The WatchPAT One is a popular at-home sleep test that helps your doctor understand how you breathe and sleep during the night. It uses a small finger sensor, a wrist monitor, and a chest sensor to track your oxygen levels, breathing patterns, snoring, and sleep position while you sleep in your own bed. The test has been shown to closely match results from an in-lab sleep study. It is a one-time-use device, so there’s nothing to return after the test. The WatchPAT One can accurately detect different types of sleep apnea, helping your doctor determine the right treatment for you.
- The NightOwl is a small, comfortable sensor worn on your fingertip that helps your doctor understand your breathing during sleep. It can be worn for several nights, allowing it to capture changes in your sleep from night to night for a more complete picture. While you sleep at home, it tracks your oxygen levels, heart rate, and breathing patterns. The NightOwl is a disposable device, so there’s nothing to return after testing, making the process simple and convenient.
The choice of device often depends on what your provider or telehealth service uses. All FDA-cleared devices meet clinical effectiveness standards, so the most important factor is following the instructions carefully to ensure accurate data collection.
Insurance Coverage and Costs
Understanding the financial aspects of home sleep testing helps you plan appropriately and take advantage of available coverage.
Medicare Part B covers home sleep tests (Types II, III, and IV) when ordered by your physician and medically necessary for diagnosing obstructive sleep apnea. You must have documented symptoms and a face-to-face evaluation within 30 days of the test order. After meeting your Part B deductible ($257 in 2025), Medicare typically pays 80% of the approved amount, leaving you responsible for 20%. The Medicare-approved amount for home sleep testing is generally $150 to $300, meaning your out-of-pocket cost would be $30 to $60.
Most private insurance plans also cover home sleep testing when medically necessary. Coverage varies by plan: some require prior authorization, some have preferred providers or specific devices, and cost-sharing depends on your deductible and coinsurance. Contact your insurance company before testing to verify coverage and understand your expected costs.
Medicare Advantage plans must provide at least the same coverage as Original Medicare but may have network restrictions. Check whether your preferred provider or telehealth service is in-network to minimize costs.
For those paying out of pocket, home sleep test packages through telehealth services typically cost $150 to $300, which includes the device, physician consultation, and results interpretation. This compares favorably to in-lab polysomnography, which can cost $1,000 to $10,000 without insurance.
Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA) can be used to pay for home sleep tests, allowing you to use pre-tax dollars and effectively reduce costs by your marginal tax rate.
What Happens After Your Test?
Your home sleep test generates a detailed report that provides the information needed for diagnosis and treatment planning.
The most important number in your report is the Apnea-Hypopnea Index (AHI). This tells you how many times per hour, on average, your breathing was interrupted. An AHI below 5 is normal and indicates you do not have sleep apnea. An AHI of 5 to 14 indicates mild sleep apnea. An AHI of 15 to 29 indicates moderate sleep apnea. An AHI of 30 or higher indicates severe sleep apnea.
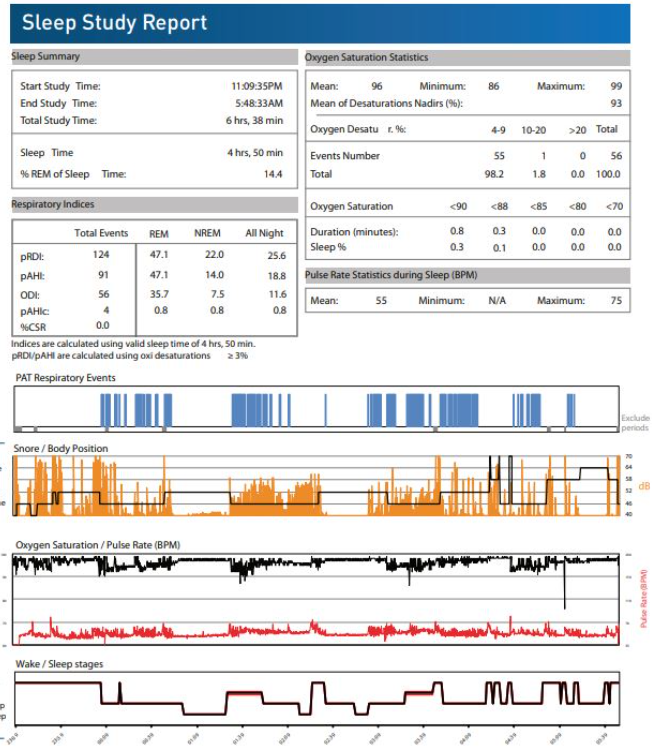
Your report will also include the Oxygen Desaturation Index (ODI), which measures how many times per hour your blood oxygen dropped significantly. Low oxygen levels during sleep contribute to the health risks associated with sleep apnea. The lowest oxygen saturation recorded during the night is also noted, with values below 88% considered clinically significant.
Depending on the device used, your report may include sleep time (actual time you were asleep versus time in bed), sleep stages (light, deep, and REM sleep), body position data (whether you had more events while sleeping on your back), snoring frequency and intensity, and heart rate patterns.
A board-certified sleep physician reviews this data and provides a clinical interpretation. If you are diagnosed with sleep apnea, they will recommend treatment options appropriate for your severity level and preferences.
Treatment Options After Diagnosis
If your home sleep test confirms sleep apnea, several effective treatment options are available.
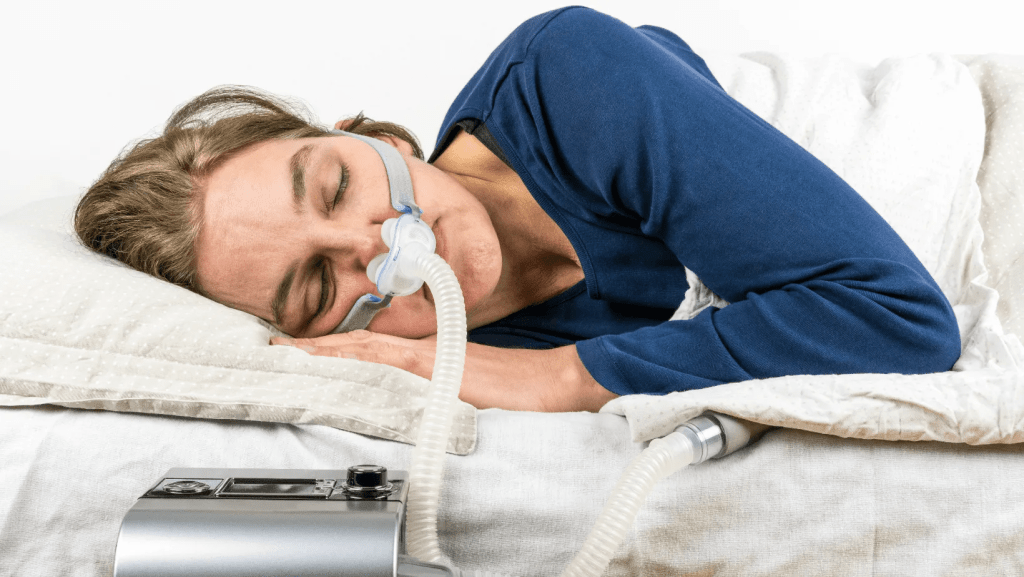
Continuous Positive Airway Pressure (CPAP) therapy remains the most effective treatment for moderate to severe obstructive sleep apnea. CPAP machines deliver a steady stream of pressurized air through a mask, keeping your airway open throughout the night. Modern CPAP machines are quieter, smaller, and more comfortable than older models. Auto-adjusting CPAP (APAP) machines automatically vary pressure based on your breathing, providing just enough support at any given moment.
Oral appliance therapy offers an alternative for mild to moderate sleep apnea or for patients who cannot tolerate CPAP. Custom-fitted mandibular advancement devices reposition your lower jaw slightly forward during sleep, tightening the soft tissues that can collapse and block your airway. These devices look similar to sports mouthguards and are fitted by dentists trained in dental sleep medicine.

Lifestyle modifications can reduce sleep apnea severity in some cases. Weight loss, if you are overweight, can significantly decrease AHI. Positional therapy (avoiding sleeping on your back) helps patients whose apnea is worse in the supine position. Avoiding alcohol and sedatives near bedtime prevents additional muscle relaxation that can worsen airway collapse.
Surgical options exist for patients with specific anatomical causes of obstruction or who have not responded to other treatments. These range from minimally invasive procedures to more extensive surgeries depending on the site and cause of obstruction.
Your physician will discuss which options are most appropriate based on your AHI, symptoms, preferences, and overall health. Many patients benefit from combining approaches, such as using an oral appliance during travel while using CPAP at home.
Home Sleep Test vs Laboratory Polysomnography
Understanding the differences between home and lab testing helps set appropriate expectations.
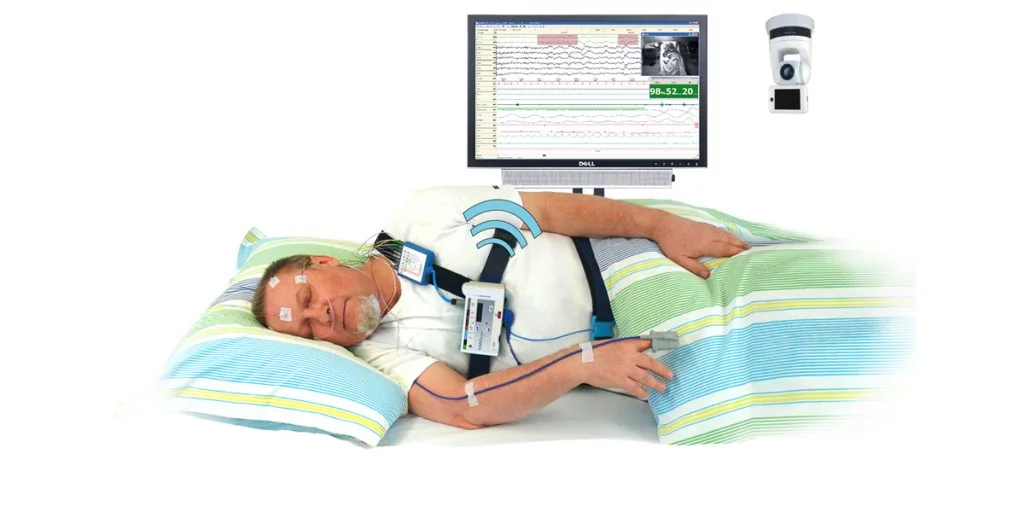
Laboratory polysomnography (PSG) is considered the “gold standard” for diagnosing sleep disorders. During a PSG, technicians monitor dozens of signals including brain waves (EEG), eye movements, chin muscle activity, leg movements, heart rhythm, breathing effort, airflow, and oxygen levels. This comprehensive monitoring can diagnose not only sleep apnea but also narcolepsy, periodic limb movements, parasomnias, and other conditions that require EEG data.
Home sleep tests are more limited in scope but highly accurate for their intended purpose: diagnosing obstructive sleep apnea. Research shows that home sleep tests achieve approximately 90% accuracy for identifying OSA, with some studies demonstrating 89% correlation with laboratory results for devices like the WatchPAT One. For most patients with classic OSA symptoms and no complicating conditions, home testing provides clinically equivalent information for diagnosis and treatment.
Home tests have inherent limitations. They may underestimate AHI by approximately 15% compared to laboratory studies because they cannot precisely measure true sleep time (only recording time).
The practical advantages of home testing are substantial. Testing in your own bed produces data more representative of your typical sleep. You avoid the discomfort and “first night effect” of sleeping in an unfamiliar lab environment. Scheduling is immediate rather than waiting weeks or months for lab availability. Costs are dramatically lower. And for many patients, the convenience of home testing means they actually complete the study rather than postponing it indefinitely.

Next Steps After Diagnosis
Receiving a sleep apnea diagnosis is not an endpoint; it is the beginning of treatment that can significantly improve your quality of life.
If diagnosed with mild sleep apnea and your symptoms are minimal, your provider may recommend lifestyle modifications as a first step, with follow-up testing after weight loss or other changes.
If diagnosed with moderate to severe sleep apnea, starting treatment promptly is important. Untreated sleep apnea is associated with increased risk of high blood pressure, heart disease, stroke, diabetes, and accidents due to daytime sleepiness. Your home sleep test prescription often translates directly to a treatment prescription: CPAP therapy is typically authorized when your AHI meets diagnostic thresholds.
For CPAP therapy, your next step is obtaining a machine and mask. Many telehealth services that provide home sleep tests also offer CPAP equipment, allowing you to move seamlessly from diagnosis to treatment. Insurance coverage for CPAP generally requires documented sleep apnea diagnosis and, for Medicare, demonstrated compliance during a 90-day trial period.
Regular follow-up matters. Modern CPAP machines track your nightly usage and effectiveness, transmitting data to cloud platforms that allow providers to monitor your progress remotely. This data also satisfies compliance requirements for ongoing insurance coverage.
Taking the first step, getting tested, is often the hardest part. Once you have a diagnosis, effective treatment is available and accessible. Many patients describe the transformation after beginning treatment as life-changing: better sleep, more energy, clearer thinking, and reduced health risks.
Frequently Asked Questions
Do I need a prescription for a home sleep test?
A prescription from a licensed healthcare provider is required to obtain most home sleep tests and to receive clinical interpretation of results. Telehealth services include physician consultation as part of their packages, making the prescription process seamless.
You can book your home sleep test with SLIIIP here.
How much does a home sleep test cost without insurance?
Complete home sleep test packages through telehealth services typically cost $150 to $300, including the device, physician consultation, and results interpretation. This is significantly less than in-lab polysomnography, which can cost $1,000 to $10,000.
Does Medicare cover home sleep tests?
Yes, Medicare Part B covers home sleep tests when ordered by a physician and medically necessary. After meeting your Part B deductible, Medicare pays 80% of the approved amount, leaving you responsible for 20%. Your out-of-pocket cost is typically $30 to $60.
How accurate are home sleep tests compared to lab studies?
Home sleep tests achieve approximately 90% accuracy for diagnosing obstructive sleep apnea, with some devices showing 89% correlation with laboratory polysomnography. They may underestimate AHI by about 15% because they cannot precisely measure true sleep time.
What if my home sleep test shows I do not have sleep apnea but I still have symptoms?
If your test is negative but symptoms persist, your provider may recommend a laboratory polysomnography. Home tests can produce false negatives in some cases, particularly for patients who did not sleep well during the test night or who have mild apnea that falls below detection thresholds.
Can I take a home sleep test if I work night shifts?
Yes, you can take the test during your normal sleep period, even if that is during daytime hours. The device records whenever you sleep, regardless of clock time.
How long does it take to get results?
Most telehealth services provide results within 1 to 7 business days after receiving your completed test data. Some cloud-based systems upload data immediately upon test completion, with physician interpretation following within 1 to 3 business days.
What is the Apnea-Hypopnea Index?
The AHI measures how many times per hour your breathing stops (apnea) or becomes significantly shallow (hypopnea) during sleep. An AHI below 5 is normal. Scores of 5 to 14 indicate mild sleep apnea, 15 to 29 indicate moderate, and 30 or higher indicate severe sleep apnea.
Can children take home sleep tests?
Most home sleep devices are validated only for adults. Children typically require laboratory polysomnography. Some devices have FDA clearance for adolescents aged 12 and older, but pediatric cases should be evaluated by a specialist.
What happens if I do not sleep well during the test?
You need at least four consecutive hours of valid data for interpretation. If technical issues or poor sleep quality affect data quality, most services offer free retesting. Multi-night devices can capture additional nights to compensate for one poor night.
Can I use HSA or FSA funds for a home sleep test?
Yes, home sleep tests qualify as eligible medical expenses for Health Savings Accounts and Flexible Spending Accounts. Using pre-tax dollars effectively reduces your cost by your marginal tax rate.
What devices do home sleep tests use?
Common FDA-cleared devices include the WatchPAT One (wrist, finger, and chest sensors), NightOwl (fingertip sensor), and Sleep Image Ring
Can a home sleep test diagnose conditions other than sleep apnea?
Home sleep tests are specifically designed to diagnose obstructive sleep apnea. They cannot diagnose narcolepsy, restless leg syndrome, periodic limb movement disorder, or parasomnias, which require the brain wave monitoring available only through laboratory polysomnography.
Do I have to return the device after my test?
It depends on the device. Disposable devices like the NightOwl are discarded after use. Reusable devices must be returned, usually via a prepaid shipping label. Check your specific instructions.
What should I do to avoid the night of my sleep test?
Avoid alcohol and sleep medications unless specifically instructed by your physician. These substances can alter your breathing patterns and produce results that do not reflect your typical sleep. Follow your normal bedtime routine otherwise.
How soon can I start CPAP therapy after diagnosis?
If diagnosed with sleep apnea that warrants CPAP, you can often begin therapy within days. Many telehealth services offer CPAP equipment directly, and prescriptions can be transmitted electronically to equipment suppliers.
Will my insurance cover CPAP if diagnosed by a home sleep test?
Yes, insurance companies accept home sleep test diagnoses for CPAP coverage authorization. Medicare and most private insurers cover CPAP when you have documented sleep apnea meeting their criteria (typically AHI of 5 or higher with symptoms, or AHI of 15 or higher regardless of symptoms).
Is one night of testing enough to diagnose sleep apnea?
We recommend 3 nights of testing to provide the most accurate data.
Can I travel with a home sleep test device?
Yes, home sleep tests can be taken while traveling. This can be particularly useful if your sleep environment at home differs significantly from where you spend most nights, such as frequent business travelers who want to test in their typical hotel environment.
What happens if I am diagnosed with central sleep apnea?
Some home sleep devices, like the WatchPAT, can detect central sleep apnea events. If central apnea is identified, your provider may recommend additional evaluation or different treatment approaches, as CPAP is primarily designed for obstructive sleep apnea. BiPAP or adaptive servo-ventilation may be more appropriate for central apnea.
Latest posts
-
Can Depression Make You Sleep Too Much? Understanding Hypersomnia and Mood
Depression can make you sleep too much, and for many people that heavy, never-rested feeling is one of the earliest signs something deeper is going on, says Dr. Avinesh Bhar,…
-
Can Anxiety Cause Insomnia? How Worry and Sleep Loss Feed Each Other
Anxiety can cause insomnia for millions of adults who lie awake with racing thoughts, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and it remains one of the most…
-
Caffeine Cutoff By Bedtime: A Practical Guide for 9pm, 10pm, 11pm, and Midnight Sleepers
Caffeine cutoff by bedtime is rarely personalized. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Most caffeine advice gives a single…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

