👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Silent Sleep Apnea: What It Is and Why It Goes Undiagnosed
Silent sleep apnea is a form of obstructive sleep apnea that produces no audible snoring. It causes repeated breathing pauses during sleep that fragment rest, reduces oxygen levels, and drive severe daytime fatigue. Millions of adults have silent sleep apnea without knowing it, making professional evaluation the only reliable way to identify it.
This article reflects the clinical insights of Dr. Avinesh Bhar, Board Certified Sleep Physician at Sliiip.com. His work evaluating thousands of patients has revealed how often silent sleep apnea hides behind exhaustion, mood changes, and morning headaches that get attributed to everything else first.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
You do not snore. Your partner has never nudged you awake. Your doctor has never flagged a breathing concern. Yet you wake up every morning feeling like you barely slept. You push through the day on caffeine and wonder what is wrong with you.
Silent sleep apnea may be the answer no one has mentioned yet.
According to the American Academy of Sleep Medicine, an estimated 26 percent of adults between the ages of 30 and 70 have obstructive sleep apnea, and a significant portion of those cases go undiagnosed because snoring is absent.
Myth vs. Reality: Silent Sleep Apnea
Myth: If you do not snore, you do not have sleep apnea.
Reality: Snoring is one possible sign of obstructive sleep apnea, not a requirement for diagnosis. Silent sleep apnea occurs when the airway partially or fully collapses during sleep without producing the characteristic noise. The breathing pauses still happen. The oxygen drops still happen. The damage to sleep quality still happens.
Myth: Sleep apnea only affects overweight men who snore loudly.
Reality: Silent sleep apnea affects men and women across all body types. Women and lean individuals are actually more likely to have silent presentations because their apnea episodes may be shorter or accompanied by hypopneas, which are partial reductions in airflow rather than complete pauses.
What Is Silent Sleep Apnea?
Silent sleep apnea refers to obstructive sleep apnea in which the characteristic loud snoring is absent or minimal. The underlying mechanism is identical to standard obstructive sleep apnea. The soft tissues of the throat relax during sleep and partially or fully block the airway.
The difference is that not every obstruction produces sound. Some people have narrowed airways that restrict airflow without vibrating loudly.

Others have episodes classified as hypopneas, which often occur without snoring but still cause meaningful oxygen drops and sleep fragmentation.
The result is the same: repeated oxygen desaturations, sleep fragmentation, and a nervous system that never fully recovers overnight.
Why Silent Sleep Apnea Is Easily Missed
Most people associate sleep apnea with loud, disruptive snoring. When that symptom is absent, neither the person nor their doctor considers it a possibility. This creates a significant diagnostic gap that can persist for years.
Often this is the sound of sleep apnea snoring. Watch the video below.
Primary care providers often rely on patient-reported symptoms. If a patient does not complain of snoring and their bed partner has not observed breathing pauses, silent sleep apnea rarely enters the clinical conversation. The symptoms that do appear, including daytime fatigue, morning headaches, and difficulty concentrating, are attributed to stress, aging, or lifestyle.
Dr. Avinesh Bhar has evaluated patients at Sliiip.com who spent years on antidepressants, stimulants, and thyroid medications before an overnight breathing evaluation revealed the true cause of their symptoms. Silent sleep apnea was present throughout. It was never suspected because snoring was never reported.
Silent Sleep Apnea Symptoms You Cannot Ignore
Silent sleep apnea does not announce itself with snoring. It signals through subtler patterns that accumulate over time and are easy to rationalize away.
Morning exhaustion despite adequate sleep hours is the most consistent complaint. You go to bed at a reasonable hour, log seven or eight hours, and still wake up feeling unrested. That persistent gap between time in bed and how you feel is a signal worth investigating professionally.
Waking with headaches is another key marker. When oxygen levels drop repeatedly overnight, blood vessels in the brain dilate. This produces a characteristic headache that is present upon waking and typically resolves within an hour of rising. If this is your daily routine, silent sleep apnea may be the cause.
Cognitive slowness and brain fog frequently accompany silent sleep apnea. Concentration, memory retrieval, and processing speed all decline when the brain is deprived of the restorative deep sleep cycles that silent sleep apnea repeatedly fragments.
Mood instability, irritability, and low motivation are common but rarely connected to breathing. The emotional regulation centers of the brain are disproportionately affected by fragmented REM sleep, which is exactly the stage that silent sleep apnea disrupts most severely.
Waking during the night without knowing why is a classic presentation. The arousal triggered by an apnea event is often brief and forgotten immediately. The person partially wakes, the airway reopens, and they fall back asleep with no memory of the event. This may happen dozens of times per night.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.

How Breathing Disruptions Affect Your Brain and Body
Every time your airway narrows during sleep, your brain registers the change in blood oxygen and triggers a micro-arousal to restore breathing. These micro-arousals last only seconds and are rarely remembered in the morning. But they interrupt the natural progression through sleep stages that your body needs for true recovery.
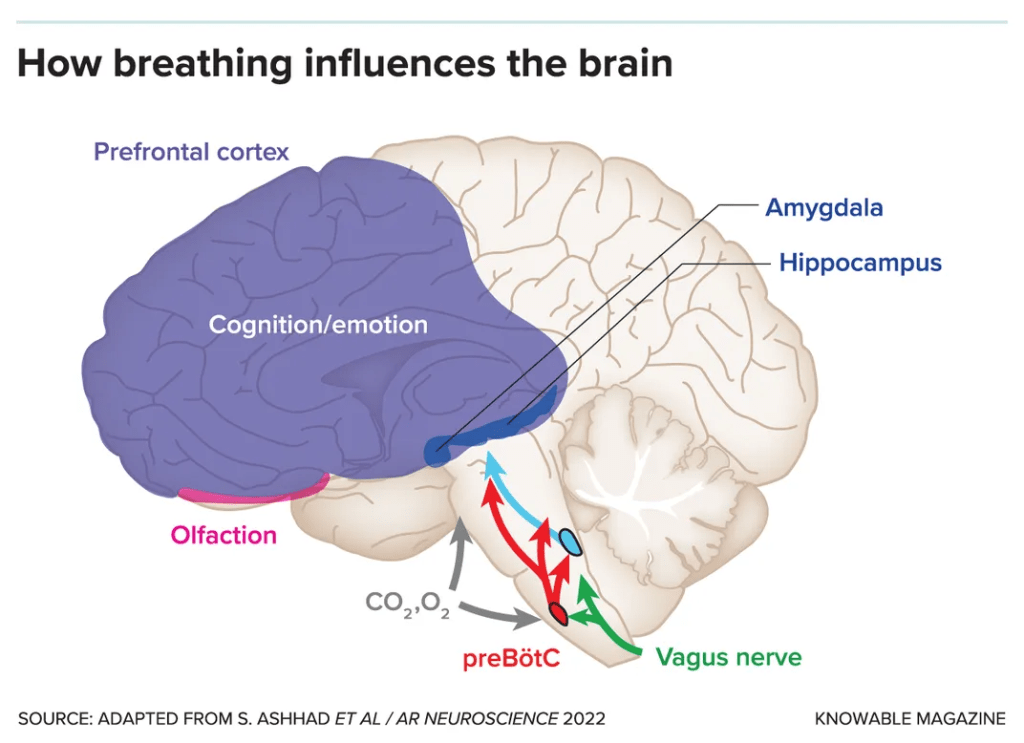
Deep slow-wave sleep, which governs physical restoration, immune function, and metabolic regulation, is repeatedly disrupted. REM sleep, which governs emotional processing and memory consolidation, is cut short. The result is a sleep structure that looks adequate on a clock but is functionally impaired.
Chronically fragmented sleep elevates cortisol, the body’s primary stress hormone. Elevated nighttime cortisol increases cardiovascular strain, promotes insulin resistance, and suppresses immune response. Research published in the American Heart Association has linked untreated obstructive sleep apnea to increased risk of hypertension, atrial fibrillation, and metabolic syndrome.
The Hidden Link Between Silent Sleep Apnea and Cardiovascular Risk
Silent sleep apnea carries the same cardiovascular risk profile as its louder counterpart. Repeated oxygen desaturations activate sympathetic nervous system pathways that raise blood pressure and increase heart rate variability overnight.
Because silent sleep apnea often goes unidentified longer than snoring presentations, the cumulative physiological exposure to these stressors may be greater.
If you have been told your blood pressure is difficult to control, or if you are experiencing fatigue with no clear explanation, sleep apnea symptoms deserve clinical attention regardless of whether snoring is present.
How Silent Sleep Apnea Is Diagnosed
The only definitive way to identify silent sleep apnea is through an overnight sleep study that measures breathing events, oxygen saturation, and sleep stages. In-laboratory polysomnography is the gold standard, but home sleep testing has become a well-validated and far more accessible alternative for most adults.
A home sleep apnea test monitors airflow, breathing effort, oxygen levels, and heart rate throughout the night. Sliiip.com ships the testing device directly to your door. The test is completed in your own bed without clinic visits. Results are reviewed by a board-certified sleep physician who can identify breathing disruptions that never produce a sound.

Expert Q&A
- How do I know I have sleep apnea?
Many patients associate sleep apnea only with loud snoring or obesity, but clinically we know:
- A significant portion of patients are undiagnosed
- Symptoms can be subtle: fatigue, headaches, poor focus, hypertension, and bruxism.
- Use chairside screening tools (STOP-BANG, Epworth Sleepiness Scale)
2) They think the oral appliance will be uncomfortable
Oral appliances (mandibular advancement devices) are custom-fit, and while it’s normal to feel some tightness at first, most patients adjust quickly.
Initial discomfort is common but usually temporary (1–3 weeks)
3) They wonder if they have to wear the oral appliance all their life?
They’ll need to use it as long as sleep apnea is present, but that doesn’t always mean forever. Changes in weight, airway anatomy, or treatment options can affect that over time.”
4) How many years can an oral appliance last?
Most appliances last several years, similar to a dental retainer. Longevity depends on wear, grinding, and maintenance.
Factors affecting lifespan:
- Bruxism (major factor)
- Material type
- Hygiene and storage
- Regular dental monitoring
5) Does insurance cover oral appliances?
In many cases, medical insurance covers oral appliance therapy for sleep apnea, especially if you’ve had a sleep study.Often requires:
- Documented diagnosis (sleep study)
- CPAP intolerance (in some plans)
- Medical necessity from sleep physicians
Rashmi Mishra – Rashmi Mishra | School of Dentistry
Frequently Asked Questions
What is silent sleep apnea?
Silent sleep apnea is obstructive sleep apnea that occurs without loud snoring. The airway still collapses repeatedly during sleep, causing oxygen drops and sleep fragmentation, but the characteristic snoring sound is absent or minimal. It is significantly underdiagnosed because most people and providers associate sleep apnea with snoring as a primary symptom.
Can you have sleep apnea without snoring?
Yes. Snoring is one possible symptom of sleep apnea, not a diagnostic requirement. Silent sleep apnea, characterized by breathing disruptions without significant noise, affects a substantial portion of people with obstructive sleep apnea. Many go undiagnosed for years because snoring is never reported.
What are the symptoms of silent sleep apnea?
Common symptoms include waking unrefreshed after a full night of sleep, morning headaches, daytime fatigue, difficulty concentrating, mood changes, irritability, and waking during the night without an obvious reason. These symptoms overlap with many other conditions, which is why silent sleep apnea is frequently attributed to stress, thyroid dysfunction, or depression.
How is silent sleep apnea diagnosed?
Diagnosis requires an overnight sleep study that measures breathing events, oxygen levels, and sleep stages. Home sleep testing is a convenient and clinically validated option for most adults. It can detect breathing disruptions regardless of whether snoring is present.
Can silent sleep apnea cause morning headaches?
Yes. Repeated overnight oxygen drops cause blood vessels in the brain to dilate, producing headaches that are typically present upon waking and resolve within an hour. This pattern is a recognized clinical marker of sleep-disordered breathing.
Is silent sleep apnea dangerous?
Untreated silent sleep apnea carries the same health risks as snoring sleep apnea, including elevated blood pressure, increased cardiovascular risk, metabolic disruption, and worsened cognitive function. Because it is diagnosed later on average, cumulative physiological exposure is often greater.
Can women have silent sleep apnea?
Yes, and women are disproportionately represented among silent sleep apnea cases. Women are more likely to present with atypical symptoms like fatigue and mood changes rather than snoring, making them particularly vulnerable to delayed diagnosis.
Does silent sleep apnea cause daytime sleepiness?
Yes. Repeated sleep fragmentation from breathing events prevents the deep restorative sleep your brain and body require. The result is excessive daytime fatigue, cognitive slowing, and reduced ability to sustain attention, even after what appears to be a full night of sleep.
Can alcohol worsen silent sleep apnea?
Yes. Alcohol relaxes the muscles of the upper airway, increasing the frequency and duration of obstructive events during sleep. Even moderate alcohol consumption in the evening can significantly worsen nighttime breathing quality for people with silent sleep apnea.
Can a home sleep test detect silent sleep apnea?
Yes. Home sleep testing measures airflow, breathing effort, oxygen saturation, and heart rate throughout the night. These measurements capture breathing disruptions regardless of whether snoring is present. A board-certified physician reviews the results to determine whether sleep-disordered breathing is occurring.
What treatments are available for silent sleep apnea?
Treatment options depend on severity and individual anatomy and may include positive airway pressure therapy, oral appliance therapy, or positional therapy. A board-certified sleep physician can recommend the most appropriate approach following a diagnostic evaluation. Learn more about oral appliance therapy.
Is silent sleep apnea related to high blood pressure?
Research from the American Heart Association supports a strong association between untreated sleep-disordered breathing and hypertension. Repeated oxygen desaturations activate pathways that elevate blood pressure overnight and during the day. If your blood pressure is difficult to control without a clear explanation, silent sleep apnea deserves clinical evaluation.
Latest posts
-
Digital Insomnia Therapy: A Doctor’s Guide to the Drug-Free Fix for Sleepless Nights
Digital insomnia therapy has quietly become one of the most effective tools in modern sleep medicine, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and many people now use…
-
AI Powered Apps for Sleep: A Doctor’s Guide to the Best Tools on Your Phone
AI powered apps for sleep now sit on more than half a billion phones around the world, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and patients walk into…
-
AI for Sleep: How Artificial Intelligence Is Changing the Way We Rest
AI for sleep has become a quiet revolution in how people fall asleep, stay asleep, and figure out what is wrong with their nights, says Dr. Avinesh Bhar, Board-Certified Sleep…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

