👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

What Causes Sleep Apnea?
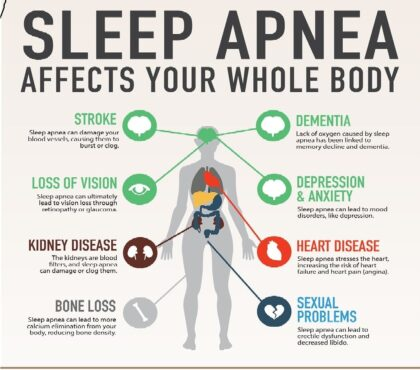
You might not remember it happening. You were asleep, after all. But somewhere during the night, your breathing paused, your body jolted awake for a fraction of a second, and then you drifted back to sleep, only for the cycle to repeat. This is the reality of sleep apnea, a condition that affects an estimated one billion people around the world. You may wonder “what causes sleep apnea?”.
Dr. Avinesh Bhar, the Founder of SLIIIP, is also a sleep apnea sufferer. He has helped thousands of patients get the evaluation and care they need, and he and his team of board-certified sleep medicine physicians can help you too. This guide breaks down everything you need to know about what causes sleep apnea, so you can better understand the condition and take the right next step.
The Two Main Types of Sleep Apnea and How They Differ
Sleep apnea falls into two primary categories, and each one has a different underlying mechanism. Obstructive sleep apnea, known as OSA, is by far the most common form. It occurs when the muscles in the back of the throat relax during sleep, allowing the surrounding soft tissue to collapse and partially or fully block the upper airway. When that happens, airflow is reduced or stopped entirely, and your body briefly wakes itself up to restore normal breathing. If you are wondering whether you might recognize some of the common signs of sleep apnea, this pattern of repeated airway blockage is at the heart of OSA.
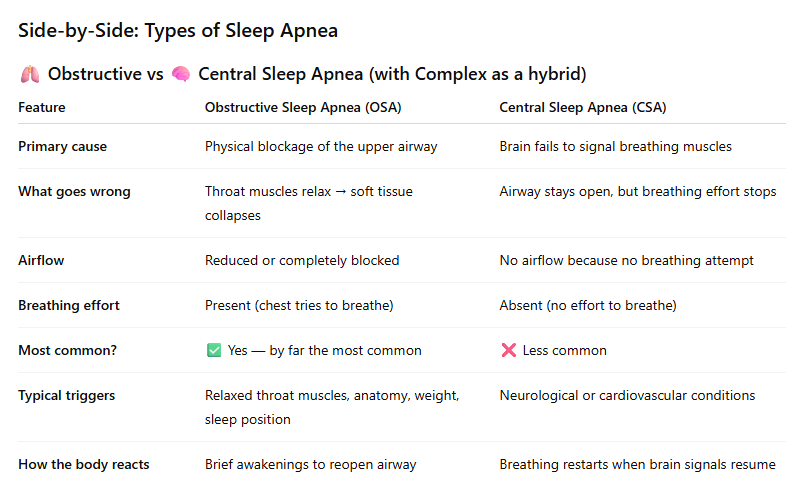

Central sleep apnea, or CSA, is less common and works very differently. Rather than a physical obstruction, central sleep apnea occurs when the brain temporarily fails to send the correct signals to the muscles that control breathing. The airway itself may remain open, but the body simply does not attempt to breathe for a brief period. This type is often connected to other health conditions that affect the central nervous system.
There is also a third category called complex sleep apnea, sometimes referred to as treatment-emergent central sleep apnea. This occurs when someone being addressed for obstructive sleep apnea with a CPAP machine develops central apnea events during the process. It is relatively uncommon, but it highlights the complexity of this condition. You can learn more about the broader picture of this condition in this overview of what sleep apnea is.
Physical and Anatomical Factors Behind Obstructive Sleep Apnea
The causes of obstructive sleep apnea are largely structural. Anything that narrows the upper airway or makes it more prone to collapsing during sleep can contribute to the condition. One of the most well-documented factors is excess body weight. Fat deposits around the neck and throat can press on the airway, making it more likely to close during the muscle relaxation that naturally occurs during sleep. According to the National Heart, Lung, and Blood Institute, maintaining a healthy weight can help reduce this particular risk factor. If you are curious about the relationship between body composition and sleep apnea, SLIIIP has explored whether being overweight can contribute to sleep apnea in more detail.
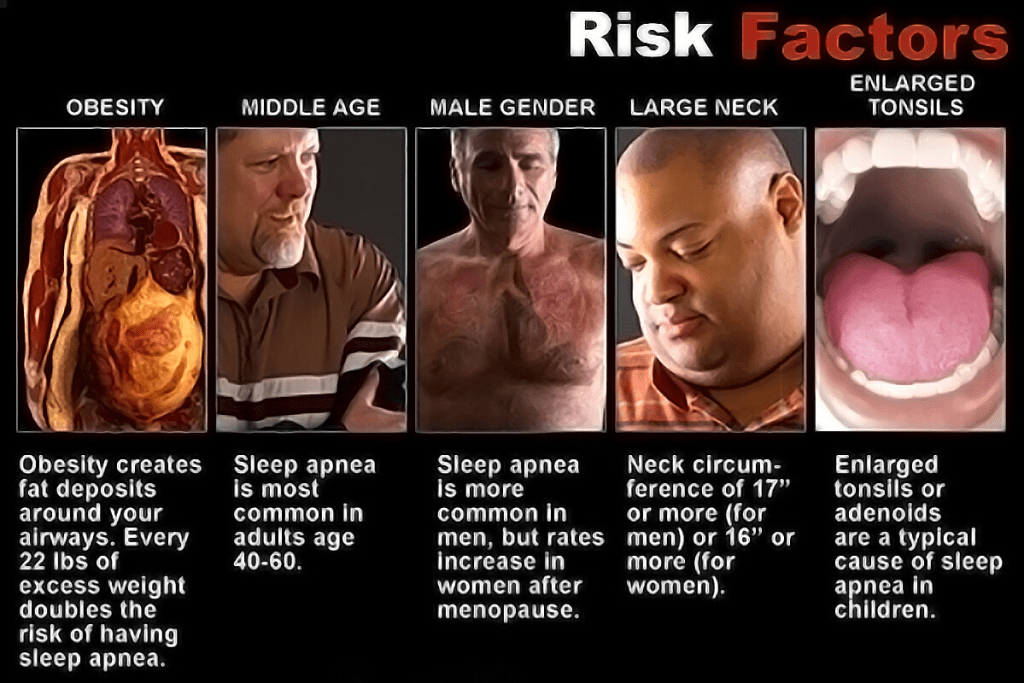
Beyond weight, the physical structure of your face, jaw, and throat plays a significant role. Some people are born with a naturally narrow airway. Others may have a larger tongue, enlarged tonsils or adenoids, or a soft palate that sits lower in the throat. These features can make the airway more vulnerable to collapse, even in people who are otherwise at a healthy weight. Craniofacial characteristics such as a receding chin or a smaller lower jaw are also recognized contributors.
Neck circumference is another factor that healthcare providers often consider. A thicker neck may indicate a narrower airway, which is one reason why this measurement is sometimes included in sleep apnea screenings.
Lifestyle Habits That Can Increase the Risk
While anatomy plays a large role, certain lifestyle habits can make obstructive sleep apnea worse, or even contribute to its development. Alcohol consumption is one of the most commonly cited factors. Alcohol relaxes the muscles of the throat and mouth, making it easier for the airway to collapse during sleep. This is why snoring and breathing disruptions are often worse on nights when alcohol has been consumed, especially close to bedtime.
Smoking is another factor. It can cause inflammation and fluid retention in the upper airway, which narrows the passage through which air flows. People who smoke have a higher likelihood of developing obstructive sleep apnea compared to those who do not.
Sedative medications, including certain anti-anxiety drugs and sleeping pills, work similarly to alcohol by relaxing the muscles in the throat. If you are taking any of these medications and have concerns about your breathing during sleep, it may be worth discussing with a healthcare provider.
Sleep position also matters. Sleeping on your back allows gravity to pull the tongue and soft tissues backward, which can narrow or block the airway more easily than sleeping on your side. SLIIIP has looked at the connection between sleep position and sleep apnea for those who want to explore this topic further.
Book a Sleep Evaluation With Our Board-Certified Sleep Doctors
SLIIIP’s team of board-certified sleep medicine physicians is licensed in 40 states and ready to help. No referral needed. No long waits. Consultations happen from the comfort of your home via telemedicine.
We can help with: Obstructive Sleep Apnea, Central Sleep Apnea, Snoring, CPAP Therapy and Management, Oral Appliance Therapy, Home Sleep Testing, Chronic Fatigue and Daytime Sleepiness, Sleep-Related Breathing Disorders.
We accept Medicare, Tricare, and most major insurance plans. Book your appointment today.
Age, Sex, and Genetics as Contributing Factors
Some risk factors for sleep apnea are simply beyond your control. Age is one of the most significant. As we get older, the muscles in the throat naturally lose some of their tone and firmness, which can increase the likelihood of airway collapse during sleep. Sleep apnea is most commonly identified in adults over the age of 50, though it can occur at any age, including in children.
Sex is another factor. Men are roughly twice as likely as women to develop obstructive sleep apnea. However, this gap narrows significantly after menopause, when hormonal changes can alter the shape and tone of the upper airway. Women are also more likely to experience subtler symptoms, which can make the condition harder to identify. For a closer look at how sleep apnea affects different groups, you can read the complete guide to sleep apnea.

Family history and genetics play a role as well. The size and shape of your skull, jaw, and airway are partly determined by your genes. If close family members have been identified as having sleep apnea, your own risk may be higher. Certain genetic conditions, including Down syndrome and cleft palate, are also associated with a greater likelihood of developing the condition.
Medical Conditions That Can Cause or Worsen Sleep Apnea
🦋 Endocrine & Hormonal Conditions
☐ Hypothyroidism – Can contribute to airway narrowing
☐ Polycystic Ovary Syndrome (PCOS) – Hormonal imbalance linked to airway changes
☐ Acromegaly – Enlarged tongue and soft tissues increase obstruction risk
☐ Pregnancy-related hormonal changes – Can raise sleep apnea risk during pregnancy
→ Covered by SLIIIP in discussions on sleep challenges during pregnancy
❤️ Cardiovascular & Fluid-Related Conditions
☐ Heart failure – Fluid shifts toward the neck when lying down
☐ Kidney failure – Fluid retention increases airway pressure during sleep
☐ Fluid redistribution when supine – Neck tissue compression of the airway
☐ Coexisting cardiovascular disease – Frequently overlaps with sleep apnea
🧠 Neurological Conditions (Central Sleep Apnea)
☐ Heart failure (CSA association) – One of the most common drivers of CSA
☐ Stroke – Can disrupt brainstem breathing control
☐ Amyotrophic lateral sclerosis (ALS) – Affects respiratory muscle signaling
☐ Myasthenia gravis – Weakens muscles involved in breathing
☐ Long-term opioid use – Suppresses the brain’s breathing regulation during sleep
Why Sleep Apnea Often Goes Unrecognized
One of the most challenging aspects of sleep apnea is that many people do not realize they have it. Because the breathing pauses and brief awakenings happen during sleep, you may not remember them at all. It is often a partner, family member, or roommate who first notices loud snoring, gasping, or periods of silence during the night.
Daytime symptoms can also be easy to dismiss. Feeling tired after a full night of sleep, struggling with focus and concentration, waking with a headache, or feeling unusually irritable are all potential indicators, but they are commonly attributed to stress, aging, or a busy schedule. If you frequently sleep eight hours and still feel tired, it may be worth exploring whether disrupted breathing during the night is playing a role. The experience of brain fog related to sleep apnea is another common but often overlooked signal.
An estimated 80 percent of people with obstructive sleep apnea remain unaware of their condition. This gap between prevalence and awareness is one of the reasons why education around the causes and signs of sleep apnea is so important.
How Sleep Apnea Is Identified
A sleep study is the standard method for identifying sleep apnea. During a sleep study, your breathing patterns, heart rate, blood oxygen levels, and other body functions are monitored while you sleep. This can be done at a sleep laboratory or, increasingly, through a home sleep apnea test. Home-based tests use portable devices to track your breathing and oxygen levels from the comfort of your own bed, and they are a practical option for many people.
The results of a sleep study include your apnea-hypopnea index, or AHI, which measures how many times per hour your breathing slows or stops during sleep. This number helps healthcare providers determine the presence and severity of the condition. If you are considering taking the first step, SLIIIP offers a sleep apnea quiz that can help you evaluate whether further evaluation may be appropriate. You can also learn more about how to get a home sleep test through SLIIIP’s step-by-step guide.
Approaches That May Help Address the Causes
Because the causes of sleep apnea are so varied, the approaches to managing it are equally diverse. For people whose condition is related to excess weight, working toward a healthy body composition can make a meaningful difference. Even modest changes can reduce fat deposits around the airway and improve airflow during sleep. SLIIIP has explored the connection between weight management and sleep apnea for those interested in this path.
CPAP therapy remains one of the most widely recognized options for managing moderate to severe obstructive sleep apnea. A CPAP machine delivers a steady stream of air through a mask to keep the airway open during sleep. For those who find CPAP challenging to use consistently, oral appliances offer an alternative. These custom-fitted devices work by repositioning the jaw or tongue to help keep the airway clear. You can explore the top-rated oral appliances for sleep apnea to understand the options available.
Lifestyle adjustments such as reducing alcohol intake, avoiding sedatives before bed, and adjusting your sleep position can also help reduce the frequency of breathing disruptions. Building a consistent sleep routine is another supportive step that many people find beneficial.
For central sleep apnea, the approach often focuses on addressing the underlying condition, whether that involves optimizing care for heart failure, adjusting medications, or using specialized positive airway pressure devices that adapt to the person’s breathing patterns.
When to Seek Professional Guidance
If you or someone close to you has noticed signs like loud snoring, choking episodes during sleep, excessive daytime fatigue, or morning headaches, it is a good idea to speak with a healthcare provider. A specialist sleep doctor can help determine whether a sleep study is appropriate and guide you through the process of understanding what is happening during the night.
Sleep apnea is a condition that develops for a variety of reasons, and no two people experience it in exactly the same way. But the underlying causes are well understood, and the options for addressing them continue to improve. Whether the root is physical, neurological, or lifestyle-related, understanding the cause is the foundation for taking the next step.
Ready to Find Out What Is Causing Your Sleep Problems?
SLIIIP’s board-certified sleep medicine physicians are licensed in 40 states and specialize in identifying the root cause of your sleep difficulties. Get evaluated from home with no referral required.
We can help with: Sleep Apnea Evaluation and Diagnosis, Home Sleep Testing, CPAP Setup and Ongoing Management, Oral Appliance Therapy, Snoring, Excessive Daytime Sleepiness, Sleep-Related Cardiovascular Concerns.
We accept Medicare, Tricare, and most major insurance plans. Schedule your evaluation now.
Frequently Asked Questions About What Causes Sleep Apnea
What is the most common cause of sleep apnea?
The most common cause of obstructive sleep apnea is the relaxation of throat muscles during sleep, which allows the surrounding soft tissue to collapse and block the airway. Excess body weight, which increases fat deposits around the neck and tongue, is one of the most significant contributing factors.
Can you develop sleep apnea at any age?
Yes, sleep apnea can develop at any age, including in children. However, the risk increases with age, and it is most commonly identified in adults over the age of 50. In children, enlarged tonsils or adenoids are a frequent cause.
Does weight always cause sleep apnea?
No. While excess weight is one of the most well-documented risk factors, many people with sleep apnea are at a healthy weight. Anatomical features like a narrow airway, a large tongue, or a receding jaw can also lead to the condition.
Is sleep apnea genetic?
There is a genetic component. The size and shape of your skull, jaw, and airway are partly inherited, so having close family members with sleep apnea can increase your own risk.
Can alcohol cause sleep apnea?
Alcohol does not directly cause sleep apnea, but it can significantly worsen it. Alcohol relaxes the muscles in the throat, making the airway more prone to collapse during sleep. Avoiding alcohol in the hours before bedtime can help reduce breathing disruptions.
Why is sleep apnea more common in men?
Men tend to have larger neck circumferences and different fat distribution patterns than women, both of which increase the risk of airway collapse during sleep. Hormonal differences also play a role, though women’s risk increases after menopause.
Can nasal congestion cause sleep apnea?
Chronic nasal congestion, whether from allergies, a deviated septum, or other structural issues, can make it harder to breathe through the nose and increase the likelihood of airway obstruction during sleep.
What is the difference between obstructive and central sleep apnea?
Obstructive sleep apnea is caused by a physical blockage of the airway, typically from relaxed throat muscles and soft tissue. Central sleep apnea occurs when the brain does not send the proper signals to the muscles that control breathing.
Can heart problems cause sleep apnea?
Heart failure is one of the most commonly associated conditions with central sleep apnea. Fluid buildup from heart or kidney failure can also shift to the neck area when lying down, contributing to airway obstruction.
Does smoking increase the risk of sleep apnea?
Yes. Smoking causes inflammation and fluid retention in the upper airway, which can narrow the breathing passage and increase the likelihood of developing obstructive sleep apnea.
Can sleep position affect sleep apnea?
Sleeping on your back allows gravity to pull the tongue and soft tissues backward, which can narrow or block the airway. Sleeping on your side is generally associated with fewer breathing disruptions.
Do children get sleep apnea?
Yes. In children, the most common cause of obstructive sleep apnea is enlarged tonsils or adenoids. Childhood obesity and certain craniofacial conditions can also contribute.
Can sleep apnea develop during pregnancy?
Hormonal changes, weight gain, and fluid retention during pregnancy can all increase the risk of developing or worsening sleep apnea. This is particularly relevant during the later stages of pregnancy.
Is sleep apnea caused by stress?
Stress itself does not directly cause sleep apnea, but it can contribute to poor sleep habits, weight gain, and increased alcohol consumption, all of which are risk factors for the condition.
Can thyroid problems cause sleep apnea?
Yes. Hypothyroidism can affect the size and tone of the muscles in the throat and tongue, increasing the risk of airway collapse during sleep.
What role do hormones play in sleep apnea?
Hormones influence the size, shape, and muscle tone of the upper airway. Conditions like PCOS, hypothyroidism, and menopause can all alter hormone levels in ways that increase the risk of sleep apnea.
Can medications cause sleep apnea?
Certain medications, particularly opioids, sedatives, and muscle relaxants, can interfere with the brain’s control of breathing or relax the throat muscles enough to increase the risk of sleep apnea.
Is sleep apnea permanent?
Sleep apnea is a chronic condition, but it can be effectively managed. In some cases, addressing the underlying cause, such as achieving a healthier body weight, can significantly reduce or resolve the condition.
How do I know if my snoring is caused by sleep apnea?
Not all snoring indicates sleep apnea. However, if snoring is accompanied by witnessed breathing pauses, gasping, excessive daytime sleepiness, or morning headaches, a sleep study can help determine whether sleep apnea is present.
Can sleep apnea cause other health problems?
Untreated sleep apnea is associated with a range of health concerns, including high blood pressure, irregular heart rhythms, type 2 diabetes, and increased daytime fatigue. Identifying and managing the condition can help reduce these associated risks.
Latest posts
-
Why is my sleep getting worse as I get older?
A serious sleep problem is often overlooked. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
How to Know If You Have a Serious Sleep Problem or a Temporary One
A serious sleep problem is often overlooked, according to Dr. Avinesh Bhar Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
Why Do I Wake Up Feeling Worse Than When I Went to Bed? What Waking Up Tired Is Really Telling You
Waking up tired is one of the most common complaints patients bring into the exam room, and it is also one of the most misunderstood, says Dr. Avinesh Bhar, Board-Certified…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

