
Why can’t I fall asleep even when I’m tired?
You have been running on fumes all day. Your eyelids are heavy. Every part of you feels drained. You crawl into bed, ready for sleep to take over, and then… nothing. You lie there, wide awake, and you wonder “why can’t I fall asleep even when I’m tired.”
In this article, Dr. Avinesh Bhar explores why your body fights sleep even when you are exhausted. He is the Founder of SLIIIP and also a board-certified physician. He and his team has helped thousands of people in 2025 sleep better through treatment methods approved by insurances.
The Science Behind Being Tired But Unable to Sleep
The longer you are awake, the stronger the urge to sleep becomes. At the same time, your nervous system needs to shift from its daytime “alert” mode (sympathetic activation) to its nighttime “rest” mode (parasympathetic activation).
When you are tired but cannot sleep, it usually means one of these systems is out of sync. You may have plenty of sleep pressure, but your nervous system is stuck in a heightened state that prevents you from relaxing enough to fall asleep. This is the “tired but wired” phenomenon, and it has real physiological explanations.
Common Reasons You Cannot Fall Asleep When You Are Tired
1. Stress and an Overactive Mind
Stress is the single most common cause of difficulty falling asleep. When you are under chronic stress, your body produces elevated levels of cortisol and adrenaline, stress hormones that keep your nervous system in fight-or-flight mode. During the day, you may be too busy to notice. But at night, when external distractions disappear, the stress response takes center stage. Your mind races, your muscles tense, and your body simply cannot relax enough to fall asleep.
2. Anxiety and Sleep-Onset Worry
Anxiety about sleep itself can become its own problem. If you have experienced multiple nights of difficulty falling asleep, your brain may begin to associate the bed with frustration and wakefulness rather than rest. This is called conditioned insomnia and it creates a self-reinforcing loop: you worry about not sleeping, which activates your stress response, which keeps you awake. Understanding the different types of insomnia can help clarify whether this pattern applies to you.

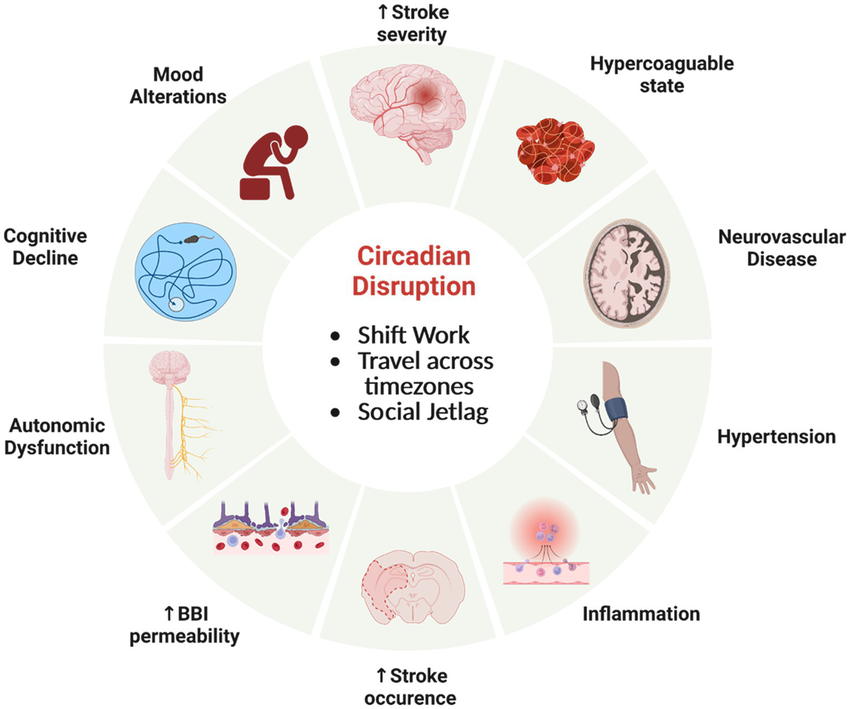
3. Circadian Rhythm Misalignment
Your internal body clock, known as your circadian rhythm, controls the timing of when you feel sleepy and when you feel alert. If your rhythm is out of sync with your schedule, perhaps from irregular sleep hours, shift work, jet lag, or excessive screen time at night, you may feel physically tired but your brain’s clock has not yet sent the signal to initiate sleep. This is especially common in people who stay up late on weekends and then try to return to an earlier bedtime during the week.
4. Caffeine and Stimulant Effects
Caffeine has a highly variable half-life, ranging from approximately 2 to 10 hours depending on individual factors, meaning that a significant portion of your afternoon coffee may still be circulating in your system at bedtime. Even if you feel tired, the caffeine is blocking adenosine receptors in your brain, the very receptors that signal sleepiness. Many people underestimate how long caffeine affects them, especially as they age and caffeine metabolism slows.
5. Screen Time and Blue Light Exposure
Electronic screens emit blue light that suppresses melatonin production. Melatonin is the hormone your brain releases in response to darkness, signaling that it is time to sleep. When you scroll through your phone or watch television in bed, you are essentially telling your brain to stay alert even as the rest of your body is begging for rest.
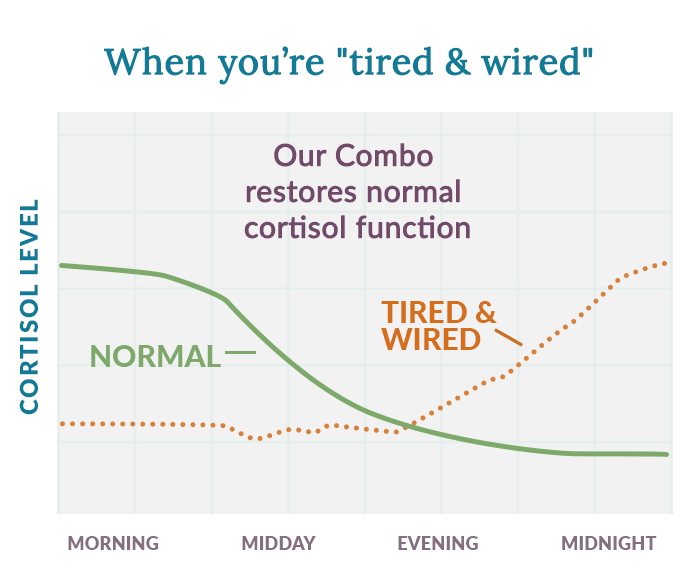
6. Overtiredness and the Cortisol Paradox
It sounds counterintuitive, but being too tired can actually make it harder to fall asleep. When you push past your natural sleep window, your body can trigger a second wind by releasing cortisol and adrenaline to keep you functioning.
7. Undiagnosed Sleep Disorders
Conditions like obstructive sleep apnea (OSA), restless legs syndrome (RLS), and periodic limb movement disorder can all disrupt the transition into sleep. Sleep apnea, in particular, can cause a cycle where poor-quality sleep leads to daytime exhaustion, which leads to elevated stress hormones that make it difficult to fall asleep the following night. Many people with these conditions are completely unaware that their sleep is being disrupted.
Did You Know: Obstructive sleep apnea does not only affect people who snore loudly. Women, younger adults, and people at a healthy weight can all have sleep apnea. If you consistently feel tired but struggle to fall asleep, a sleep evaluation may reveal a treatable underlying cause.
8. Medical Conditions and Medications
Chronic pain, thyroid disorders (particularly hyperthyroidism), hormonal changes during menopause, and neurological conditions can all interfere with sleep onset. Additionally, certain medications, including some antidepressants, decongestants, blood pressure medications, and stimulant-based ADHD treatments, can cause insomnia as a side effect.
Self-Assessment: Is It Time to See a Sleep Specialist?
If you answer “yes” to two or more of the following, a professional sleep evaluation may help:
- You regularly take more than 30 minutes to fall asleep despite feeling tired
- You wake up feeling unrefreshed most mornings
- A bed partner has mentioned snoring, gasping, or restless movement during your sleep
- You experience daytime fatigue, brain fog, or difficulty concentrating
- You have tried improving sleep habits without significant improvement
- You feel anxious or dread bedtime because of past difficulty falling asleep

Evidence-Based Strategies to Fall Asleep When You Are Tired
Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is the gold standard treatment for chronic insomnia, recommended as a first-line therapy before medication. It works by identifying and changing the thoughts and behaviors that keep you awake. Techniques include stimulus control (only using the bed for sleep), sleep restriction (temporarily limiting time in bed to build stronger sleep drive), and cognitive restructuring (addressing unhelpful beliefs about sleep).
Consistent Sleep-Wake Schedule
Going to bed and waking up at the same time every day, including weekends, helps synchronize your circadian rhythm. If your schedule is significantly off, adjust gradually by shifting your bedtime and wake time by 15 to 30 minutes every few days. For a detailed approach, see our sleep routine guide.
Strategic Light Exposure
Get bright light exposure within 30 minutes of waking, ideally from natural sunlight for at least 10 to 15 minutes. In the evening, dim lights and avoid screens at least 30 minutes before bed to support natural melatonin production.
Relaxation Techniques
Progressive muscle relaxation, the 4-7-8 breathing technique (inhale for 4 counts, hold for 7, exhale for 8), and guided imagery have all been shown to activate the parasympathetic nervous system and help ease the transition into sleep.
Address Underlying Sleep Disorders
If a sleep study reveals obstructive sleep apnea, treatment with CPAP therapy or oral appliance therapy can resolve the underlying cause of your poor sleep, often dramatically improving both sleep quality and the ability to fall asleep. Telemedicine services like SLIIIP make it easy to consult with a board-certified sleep specialist and receive a home sleep test without delays.
Oral Appliance Therapy: What Patients Want to Know
For patients diagnosed with obstructive sleep apnea, oral appliance therapy (also known as a mandibular advancement device) is a comfortable, portable alternative to CPAP. These custom-fitted dental devices gently reposition the lower jaw forward during sleep.

Below a dentist who specializes in dental sleep medicine answer common patient questions:
Q: Is oral appliance covered by insurance and is it better than CPAP
Michael J Landry, DDS ABAD
hhsapnea.com
“Absolutely, in fact we are in medical network with BCBS, Aetna, Cigna, and Medicare.
Is it more comfortable than CPAP?
Yes, 90% of patients are still wearing their appliance one year later, while only 30% of patients who start with CPAP are wearing it at the end of a year.”
Q. How many years can an oral appliance last?
“Average is 3 years, depending on how well it is cared for.”
Frequently Asked Questions
Why am I so tired but my body will not let me sleep?
This usually means your nervous system is in a heightened state even though your body is exhausted. Stress, anxiety, caffeine, screen time, circadian rhythm disruption, and undiagnosed sleep disorders can all keep your brain’s arousal system activated, preventing the shift into sleep despite strong physical fatigue.
How long should it normally take to fall asleep?
Most healthy adults fall asleep within 10 to 20 minutes of getting into bed. Consistently taking longer than 30 minutes is considered a sign of sleep-onset difficulty and may warrant evaluation, especially if accompanied by daytime fatigue.
Can sleep apnea make it hard to fall asleep?
Yes. While sleep apnea is best known for disrupting sleep during the night, the chronic poor sleep quality it causes can lead to elevated stress hormones and nervous system hyperarousal, making it progressively harder to fall asleep over time. Treating the sleep apnea with a custom oral appliance or CPAP often resolves this issue.
Latest posts
-
Can Lack of Sleep Cause Depression?
You have been running on too little rest for weeks, maybe months. The exhaustion has settled into something deeper. It is not just tiredness anymore. The world feels grayer and…
·
-
Why Do I Feel Sad and Unmotivated When I Don’t Sleep?
You set the alarm early, planned your whole day, and still ended up lying on the couch by noon wondering what went wrong. Your to-do list sits untouched. You feel…
·
-
Is My Depression Actually a Sleep Problem?
You are exhausted all the time. You have lost interest in things you used to enjoy. Concentrating feels impossible. Your mood is flat, or worse. Your doctor diagnosed depression but…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

