👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Life Expectancy and Sleep Apnea: What the Research Shows and Why It Matters
Few questions about sleep apnea carry as much weight as this one: what is the life expectancy and sleep apnea? It is a question that deserves a thoughtful, honest answer.
Dr. Avinesh Bhar, the Founder of SLIIIP, is also a sleep apnea sufferer. He has helped thousands get evaluated and begin managing their condition, and he and his team of board-certified sleep medicine physicians can help you too. This guide breaks down everything the research shows about life expectancy and sleep apnea so you can understand the facts and take informed action.
What the Experts Say
The short version is that sleep apnea itself is not a direct cause of shortened lifespan. But the cascading effects it can have on the body, when the condition goes unrecognized and unmanaged over time, are associated with serious health considerations that can meaningfully affect long-term wellness. The encouraging part is that the same research consistently shows that proper management can make a significant difference.
What Happens to the Body During Untreated Sleep Apnea
To understand why sleep apnea is linked to long-term health concerns, it helps to understand what happens during the night in someone whose condition is not being managed. Each time breathing pauses, whether from a physical airway obstruction or a lapse in brain signaling, the oxygen level in the blood drops. The body responds with a stress reaction: a brief surge of adrenaline, an increase in heart rate, and a spike in blood pressure. These micro-awakenings happen so quickly that you typically do not remember them, but your body registers every one.

In mild cases, this might happen 5 to 14 times per hour. In severe cases, it can occur 30, 60, or even more than 100 times per hour. Over the course of a full night, that adds up to hundreds of stress responses, each one pulling the body out of restorative sleep and placing additional strain on the cardiovascular system.
Night after night, month after month, year after year, this pattern takes a cumulative toll. It is not a single dramatic event that causes concern, but rather the relentless repetition of low-level physiological stress that gradually affects the body’s systems. Understanding the signs of sleep apnea is the first step in recognizing whether this pattern might be affecting you.
What the Research Shows About Sleep Apnea and Longevity
☐ Large, long-term study evidence
- The Wisconsin Sleep Cohort Study followed 1,500+ people over 18 years
- Findings were published in the journal Sleep
☐ Higher overall risk of death with severe sleep apnea
- Severe sleep apnea was linked to a ~3× higher risk of all-cause mortality
- Results were adjusted for age, sex, and BMI
☐ Even greater risk when untreated
- When people using CPAP regularly were excluded, mortality risk rose to ~4.3×
- This suggests consistent treatment is protective
☐ Cardiovascular deaths are especially common
- 42% of deaths in people with severe sleep apnea were cardiovascular-related
- Compared to 26% in people without sleep apnea
☐ Supported by broader research
- The American Academy of Sleep Medicine reports ~17% increased mortality risk with untreated sleep apnea
☐ Impact on lifespan
- Severe, untreated obstructive sleep apnea may shorten lifespan by several years
- In extreme cases, the risk may be comparable to long-term smoking
The Cardiovascular Connection
The link between sleep apnea and cardiovascular health is one of the most thoroughly studied aspects of the condition. The repeated drops in blood oxygen and the accompanying surges in sympathetic nervous system activity contribute to sustained high blood pressure, even during waking hours.
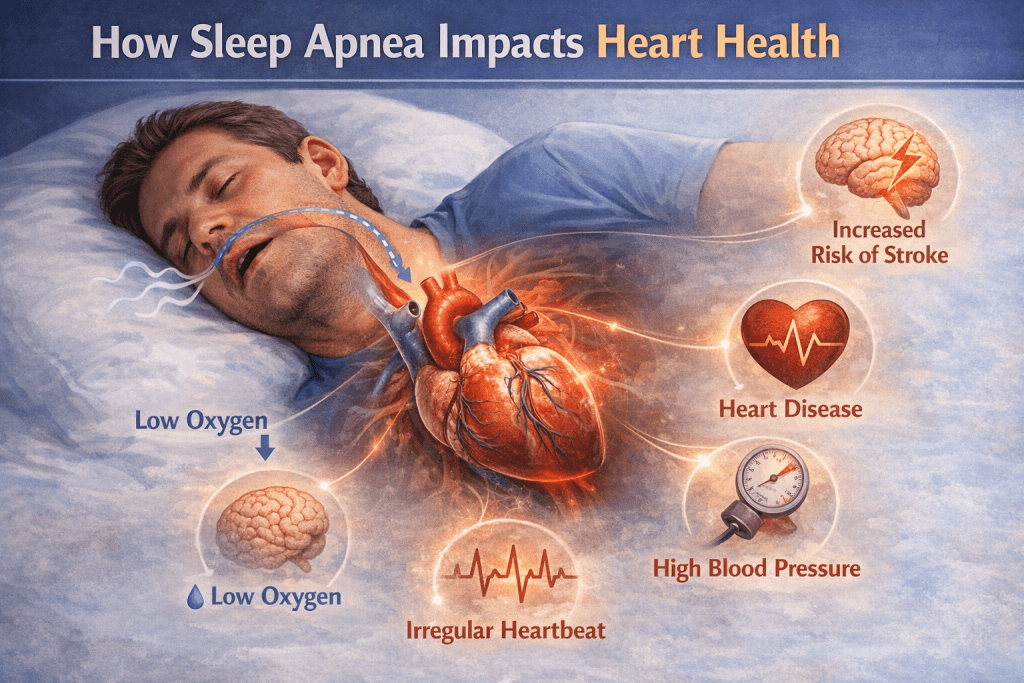
Studies have shown associations between untreated sleep apnea and several cardiovascular conditions, including hypertension, coronary artery disease, irregular heart rhythms, and stroke. The connection between sleep apnea and heart disease is well established, and the relationship between sleep apnea and atrial fibrillation has also been documented in multiple research studies.
The Johns Hopkins Medicine overview of uncontrolled sleep apnea notes that the condition is directly tied to increased cardiovascular and metabolic risk, and that many people affected are unaware they have the condition. This underscores the importance of recognizing the signs early and seeking evaluation when symptoms are present.
Metabolic and Cognitive Considerations
The impact of untreated sleep apnea extends beyond the heart. Research has shown associations with metabolic changes, including insulin resistance and an increased likelihood of type 2 diabetes. The hormonal disruptions caused by poor sleep quality can affect appetite regulation and energy metabolism, creating a cycle that makes weight management more difficult. SLIIIP has explored the relationship between sleep and weight for those interested in understanding this connection.
Cognitive function is another area of concern. Chronic sleep fragmentation affects memory consolidation, attention, and executive function. Over time, these effects can become more pronounced. The experience of brain fog related to sleep apnea is one of the most commonly reported daytime symptoms, and emerging research has begun to explore potential connections between long-term sleep apnea and cognitive decline in later life. The broader topic of how sleep relates to cognitive health is one that continues to gain attention in the research community.
Mood and mental health are also affected. The chronic fatigue and disrupted sleep associated with untreated sleep apnea can contribute to irritability, difficulty managing stress, and changes in emotional wellbeing. SLIIIP has looked at sleep solutions for mental health for those navigating this area.
Mild vs Severe: Does Severity Affect the Outlook?
The research consistently shows that severity matters. The Wisconsin Sleep Cohort Study found that the increased risk of mortality was statistically significant primarily in those with severe sleep apnea (AHI of 30 or more). Those with mild or moderate sleep apnea showed a trend toward increased risk, but the numbers did not reach statistical significance in that particular study.
This does not mean mild sleep apnea carries no long-term implications. It simply means the evidence for dramatic life expectancy effects is strongest at the severe end of the spectrum. Mild sleep apnea can still affect daily quality of life, contribute to fatigue, and potentially worsen over time if the underlying factors are not addressed. SLIIIP’s article on mild sleep apnea provides a closer look at what this level of severity means in practical terms.
For a detailed understanding of how the severity scale works and what the numbers mean, SLIIIP has a comprehensive guide on AHI scores and what they indicate.
Book a Sleep Evaluation With Our Board-Certified Sleep Doctors
SLIIIP’s team of board-certified sleep medicine physicians is licensed in 40 states and ready to help you take control of your long-term health. No referral needed. No long waits. Consultations happen from the comfort of your home via telemedicine.
We can help with: Sleep Apnea Evaluation and Diagnosis, Home Sleep Testing, CPAP Therapy and Ongoing Management, Oral Appliance Therapy, Snoring, Chronic Fatigue and Daytime Sleepiness, Sleep-Related Cardiovascular Concerns, Ongoing Remote Monitoring.
We accept Medicare, Tricare, and most major insurance plans. Book your appointment today.
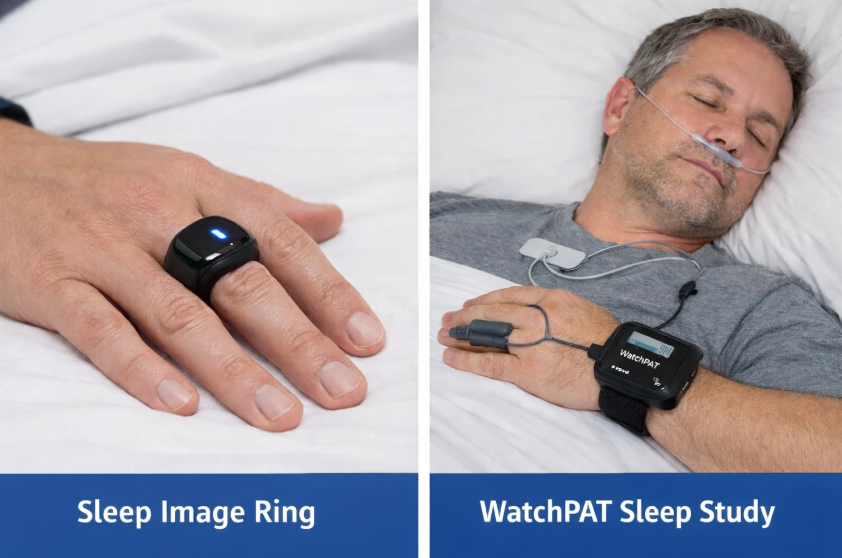
We use the Sleep Image ring and the Watch Pat for the home sleep tests and its covered by Medicare, Tricare and major health insurances.
The Impact of Management on Long-Term Outcomes
The most encouraging finding across the research is that managing sleep apnea is associated with improved outcomes. In the Wisconsin Sleep Cohort Study, the removal of consistent CPAP users from the analysis caused the mortality risk ratio to increase substantially, suggesting that regular CPAP use may offer a protective effect.
Observational studies have reported that people with sleep apnea who use CPAP consistently show lower rates of cardiovascular events, improved blood pressure control, and better overall quality of life compared to those who do not use it or use it inconsistently. While these are observational findings and not proof of direct causation, the pattern is consistent across multiple study populations.
CPAP is not the only management option. Oral appliances, which work by repositioning the jaw to keep the airway open, are an effective alternative for many people with mild to moderate sleep apnea. You can review the top-rated oral appliances available through SLIIIP. For those who find CPAP challenging, mandibular advancement devices offer another well-supported path.
Lifestyle changes also play a meaningful role. Achieving and maintaining a healthy weight can reduce the severity of obstructive sleep apnea, and SLIIIP has explored how weight management relates to sleep apnea improvement. Reducing alcohol consumption, adjusting sleep position, and building a consistent sleep routine are all supportive steps that contribute to better outcomes over time.
Biological Aging and Sleep Apnea
More recent research has begun to explore a fascinating angle: whether untreated sleep apnea accelerates the biological aging process at a cellular level. Studies examining telomere length, which is a marker of cellular aging, have found that people with untreated moderate to severe sleep apnea tend to have shorter telomeres than matched controls. One analysis estimated that severe OSA may be associated with the equivalent of approximately six additional years of biological aging.
Taking the First Step
If you have been experiencing symptoms of sleep apnea, or if a partner has noticed signs like loud snoring, choking during sleep, or observed breathing pauses, the most important thing you can do is seek evaluation. A sleep study is the standard approach for identifying sleep apnea and determining its severity.
SLIIIP makes it easy to get started with a sleep apnea quiz that can help you assess whether your symptoms suggest further evaluation. For those ready to proceed, getting a home sleep test is a convenient first step that can be done from the comfort of your own bed. SLIIIP also offers direct access to sleep telemedicine services, connecting you with healthcare providers who specialize in sleep-related concerns.
Understanding the connection between sleep apnea and long-term health is not meant to create fear. It is meant to empower informed decision-making. The research is clear that managing sleep apnea makes a difference, and the earlier you begin, the better positioned you are to support your overall wellness for the years ahead.
Take the First Step Toward Better Long-Term Health
SLIIIP’s board-certified sleep medicine physicians are licensed in 40 states and can help you get evaluated, understand your results, and build a management plan that fits your life. Get started from home with no referral required.
We can help with: Sleep Apnea Evaluation and Diagnosis, Home Sleep Testing, CPAP Therapy and Remote Monitoring, Oral Appliance Therapy, Snoring, Excessive Daytime Sleepiness, Sleep-Related Cardiovascular and Metabolic Concerns.
We accept Medicare, Tricare, and most major insurance plans. Schedule your evaluation now.
Frequently Asked Questions About Life Expectancy and Sleep Apnea
Can sleep apnea shorten your life?
Sleep apnea itself does not directly shorten life, but the health conditions it is associated with, including cardiovascular disease, high blood pressure, and metabolic disorders, can affect long-term outcomes if the condition is not managed.
How many years can untreated sleep apnea take off your life?
Estimates vary depending on severity. Some research suggests severe untreated sleep apnea may reduce lifespan by several years, with certain studies citing figures in the range of 7 to 8 years for the most severe cases. However, individual outcomes depend on many factors.
Does mild sleep apnea affect life expectancy?
The evidence for a significant impact on life expectancy is strongest for severe sleep apnea. Mild sleep apnea has a less dramatic statistical association, but it can still affect daily quality of life and may worsen over time if not addressed.
Can CPAP therapy improve life expectancy?
Observational studies suggest that consistent CPAP use is associated with lower rates of cardiovascular events and improved outcomes compared to inconsistent use or no use. While this is not definitive proof, the trend across multiple studies is encouraging.
Is severe sleep apnea dangerous?
Severe sleep apnea, with 30 or more breathing events per hour, places significant stress on the cardiovascular system. Research has shown approximately three times the all-cause mortality risk compared to people without sleep apnea, after adjusting for other factors.
What health problems are linked to untreated sleep apnea?
Untreated sleep apnea is associated with high blood pressure, heart disease, irregular heart rhythms, stroke, type 2 diabetes, weight gain, cognitive difficulties, and mood changes.
Can sleep apnea cause a heart attack?
Research has shown an association between untreated sleep apnea and increased risk of cardiac events, including heart attacks. The repeated oxygen drops and blood pressure surges during the night contribute to cardiovascular strain over time.
Does sleep apnea get worse with age?
Sleep apnea can worsen with age due to natural changes in muscle tone, weight distribution, and overall health. Regular monitoring and consistent management are important as you get older.
Can you die from sleep apnea in your sleep?
The body has protective mechanisms that trigger waking when breathing is disrupted. However, the long-term cardiovascular effects of untreated sleep apnea can increase the risk of serious events over time. Seeking evaluation and management is the most effective protective step.
Does managing sleep apnea reduce the risk of heart disease?
Observational studies have found that people who consistently manage their sleep apnea, particularly with CPAP, show lower rates of cardiovascular events and improved blood pressure compared to those who do not.
What is the mortality risk for severe sleep apnea?
The Wisconsin Sleep Cohort Study found approximately a three-fold increase in all-cause mortality risk for severe sleep apnea compared to no sleep apnea, after adjusting for age, sex, and BMI. The risk rose to approximately 4.3-fold when excluding those using CPAP.
Can weight loss improve sleep apnea and long-term health?
Yes. Weight management is one of the most effective lifestyle approaches for reducing sleep apnea severity. Even a 10 percent reduction in body weight can meaningfully reduce the AHI in many people.
Does sleep apnea affect brain health?
Chronic sleep fragmentation from untreated sleep apnea affects memory, attention, and executive function. Emerging research is also exploring potential connections between long-term untreated sleep apnea and cognitive decline in later life.
Is sleep apnea as dangerous as smoking?
Some researchers have drawn comparisons, noting that severe untreated sleep apnea may reduce lifespan by an amount approaching, though generally less than, the impact of long-term smoking. Both conditions benefit significantly from intervention.
Can young people be affected by sleep apnea and its long-term effects?
Yes. Sleep apnea can occur at any age. When present in younger adults, the cumulative effects over a longer period of time make early recognition and management particularly important.
Does sleep apnea affect blood sugar levels?
Research has shown an association between sleep apnea and insulin resistance, independent of body weight. Managing sleep apnea may help improve blood sugar regulation in some individuals.
How soon after starting management can improvements be seen?
Many people notice improvements in daytime energy, mood, and cognitive function within the first weeks of consistent management. Cardiovascular benefits are believed to accrue over longer periods of consistent use.
Can oral appliances offer the same long-term benefits as CPAP?
For mild to moderate sleep apnea, oral appliances have been shown to be effective in reducing the AHI and improving symptoms. The long-term cardiovascular data is not as extensive as for CPAP, but the evidence supports their use as a viable management option.
What should I do if I think I have sleep apnea?
The most important step is to seek evaluation. A sleep study, whether at a lab or at home, can determine whether you have sleep apnea and how severe it is. From there, you and your healthcare provider can develop a management plan tailored to your situation.
Does managing sleep apnea reverse the damage already done?
While managing sleep apnea can halt the ongoing strain on the body and reduce future risk, the extent to which existing changes can be reversed depends on individual factors and how long the condition went unmanaged. The sooner management begins, the better the overall outlook.
Latest posts
-
Why is my sleep getting worse as I get older?
A serious sleep problem is often overlooked. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
How to Know If You Have a Serious Sleep Problem or a Temporary One
A serious sleep problem is often overlooked, according to Dr. Avinesh Bhar Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Many people brush off poor sleep…
-
Why Do I Wake Up Feeling Worse Than When I Went to Bed? What Waking Up Tired Is Really Telling You
Waking up tired is one of the most common complaints patients bring into the exam room, and it is also one of the most misunderstood, says Dr. Avinesh Bhar, Board-Certified…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

