👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

What You Need to Know About Testing for Sleep Apnea at Home
You have been snoring louder than usual. Or maybe your partner has noticed you gasping during the night. Dr. Avinesh Bhar, the Founder of SLIIIP, is also a sleep apnea sufferer and can explain everything on what you need to know about testing for sleep apnea at home.
He has helped thousands get tested and receive the care they need, and he and his team of board-certified sleep medicine physicians can help you too. This guide breaks down everything you need to know about home sleep apnea testing so you can take the next step with confidence.
What Is a Home Sleep Apnea Test?
A home sleep apnea test, sometimes called an HSAT or HST, is a portable monitoring device that you wear while sleeping in your own bed. It is designed to detect obstructive sleep apnea, or OSA, by tracking key breathing-related signals throughout the night.

Unlike a full overnight sleep study conducted in a lab, which monitors a wide range of signals including brain waves, muscle tone, and eye movements, a home sleep test focuses specifically on breathing patterns. It measures things like airflow through the nose, blood oxygen levels, heart rate, breathing effort, and in many devices, body position and snoring intensity.
The data collected during a single night is then reviewed by a sleep specialist, who interprets the results and determines whether a sleep apnea evaluation is warranted. According to Johns Hopkins Medicine, home sleep apnea testing is a simplified breathing monitor that can provide meaningful insights at a fraction of the cost of an in-lab study.
How Does a Home Sleep Test Work?
The process is straightforward. After a healthcare provider determines that a home sleep test is appropriate for you, the testing device is either shipped to your home or picked up from a clinic. Most devices are compact, simple to set up, and come with clear instructions.
The Equipment
While specific sensors vary by device, most home sleep tests include a nasal cannula or prong that measures airflow through the nose, a finger probe called a pulse oximeter that monitors oxygen saturation and heart rate, and one or more sensors placed on the chest or abdomen to track breathing effort. Some more advanced devices, like the WatchPAT, use a wrist-worn unit with a finger sensor and chest sensor to measure seven different physiological variables, including peripheral arterial tone, body position, heart rate, oxygen saturation, body movement, snoring, and chest motion.
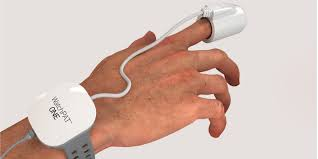
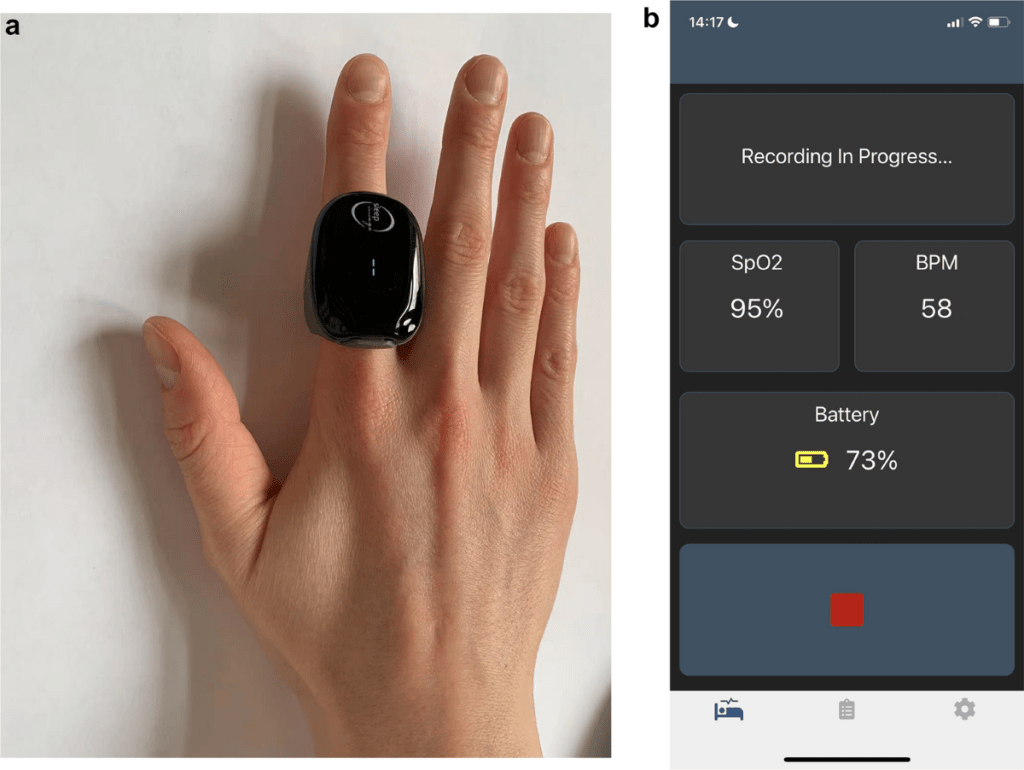
The Process
You apply the sensors before going to bed, following the provided instructions. Then you simply go to sleep as you normally would. Most home sleep tests require only a single night of data. In the morning, you remove the device and either return it to the provider or, in some cases, the data uploads automatically for review.
A sleep specialist then analyzes the recorded data and provides a report that typically includes a measurement called the Apnea-Hypopnea Index, or AHI. This number reflects how many times per hour you experienced a pause in breathing (apnea) or a significant reduction in breathing (hypopnea) during the test.

Understanding Your Results
The AHI is the primary number used to assess sleep apnea severity. Generally, an AHI of fewer than 5 events per hour is considered within the normal range. An AHI between 5 and 15 suggests mild sleep apnea, between 15 and 30 suggests moderate, and above 30 suggests severe. For a more detailed understanding of how these numbers translate to your situation, the guide on understanding AHI scores on SLIIIP provides helpful context.
Who Is a Good Candidate for a Home Sleep Test?
Home sleep apnea tests are generally recommended for adults who have a moderate to high likelihood of obstructive sleep apnea based on their symptoms and risk factors. You may be a good candidate if you experience loud snoring, your partner has observed breathing pauses or gasping during your sleep, you wake up with morning headaches or a dry mouth, or you feel excessively tired during the day despite spending enough time in bed.
If you are unsure whether your symptoms point toward sleep apnea, taking the sleep apnea quiz on SLIIIP can help you assess your risk level.
When an In-Lab Study May Be More Appropriate
While home tests are suitable for many people, there are situations where an in-lab polysomnography may be recommended instead. For a side-by-side comparison, the home vs lab sleep tests guide on SLIIIP breaks down the key differences.

Benefits of Testing at Home
There are several practical advantages to choosing a home sleep apnea test over an in-lab study.
Comfort and Convenience
Sleeping in your own bed, in your own environment, often leads to a more natural and representative night of sleep. Many people find it difficult to fall asleep in an unfamiliar lab setting, which can affect the accuracy of results. At home, you follow your normal routine, which may provide a more realistic picture of your typical sleep.
Shorter Wait Times
Sleep lab appointments can sometimes involve weeks or even months of waiting, depending on availability. Home tests can often be arranged and completed much more quickly, allowing you to get answers sooner.
Lower Cost
Home sleep tests are generally a fraction of the cost of an in-lab study. Many insurance plans cover home testing, making it an accessible option for a wider range of people. To understand more about coverage options, the article on insurance coverage for home sleep studies provides useful guidance.
Accessibility
For people who live far from a sleep center, have mobility challenges, or simply have demanding schedules, the ability to test at home removes a significant barrier to getting evaluated.
Get a Home Sleep Test Delivered to Your Door
SLIIIP’s team of board-certified sleep medicine physicians is licensed in 40 states and ready to help. No referral needed. No long waits. Your home sleep test is shipped directly to you, and consultations happen via telemedicine from the comfort of your home.
We can help with: Home Sleep Apnea Testing, Sleep Apnea Evaluation and Diagnosis, CPAP Therapy and Management, Oral Appliance Therapy, Snoring, Chronic Fatigue and Daytime Sleepiness, Sleep-Related Breathing Disorders, Ongoing Remote Monitoring.
We accept Medicare, Tricare, and most major insurance plans. Book your appointment today.
Limitations to Be Aware Of
While home sleep tests are a valuable tool, they do have some limitations that are important to understand.
Narrower Scope of Measurement
Home tests monitor breathing and oxygen levels, but they do not measure brain waves, eye movements, or leg movements. This means they cannot determine how much time you spent in different sleep stages or identify non-breathing sleep disorders. They are focused specifically on detecting obstructive sleep apnea.
Potential for Underestimation
Because most home tests do not measure actual sleep time with brain wave monitoring, they estimate sleep time using movement sensors and other indirect methods. This can sometimes lead to a reported AHI that is lower than it would be in a lab setting, where total sleep time is measured more precisely. As a result, mild cases of sleep apnea may occasionally be underdetected.
Sensor Issues
Without a technician present, there is a possibility that sensors could shift or become dislodged during the night without your awareness. Most providers report a small failure rate, typically around 7 to 8 percent, for home tests. If a test fails or produces insufficient data, a retest or in-lab study may be recommended.
How to Prepare for Your Home Sleep Test
Getting the most accurate results from your home sleep test involves a few simple preparation steps. For detailed preparation guidance, the how to prepare for a home sleep study article on SLIIIP covers everything you need to know.
In general, try to follow your usual bedtime routine on the night of the test. Avoid alcohol and caffeine in the hours leading up to sleep. Try to sleep for your usual amount of time, and aim to spend some time on both your back and your side if possible, as sleep apnea is often more pronounced when sleeping on the back.
Make sure you understand how to apply each sensor before you get into bed. Review the instructions carefully, and do not hesitate to contact the provider if anything is unclear. Proper sensor placement is the single most important factor in getting accurate results.
What Happens After the Test
Once your sleep data has been recorded and submitted, a board-certified sleep specialist reviews the results. You will typically receive a detailed report that includes your AHI, oxygen saturation levels throughout the night, and other relevant findings.
If obstructive sleep apnea is identified, your provider will discuss the findings with you and recommend next steps. These may include CPAP therapy, oral appliance therapy, lifestyle modifications, or a combination of approaches. In some cases, a follow-up in-lab study may be recommended for more detailed assessment.
If the test does not indicate sleep apnea but your symptoms persist, your provider may recommend a more comprehensive sleep evaluation to explore other possible explanations for your symptoms.
Getting Started With SLIIIP
SLIIIP makes the home sleep testing process simple and accessible. You can explore home sleep test options with a prescription or begin the process with a home sleep test assessment if you are not sure where to start. For those who need a prescription, SLIIIP also offers a pathway to get a prescription as part of the testing process.
The entire process, from ordering to results, is designed to be straightforward, with telemedicine consultations available to guide you through every step. You do not need to navigate this alone.
Ready to Find Out If You Have Sleep Apnea?
SLIIIP’s board-certified sleep medicine physicians are licensed in 40 states and make home sleep testing simple. Get your test shipped to your door, take it in your own bed, and receive expert interpretation of your results, all without leaving home.
We can help with: Home Sleep Apnea Testing, Sleep Apnea Diagnosis, CPAP Setup and Remote Monitoring, Oral Appliance Therapy, Snoring Evaluation, Excessive Daytime Sleepiness, Sleep-Related Breathing Disorders.
We accept Medicare, Tricare, and most major insurance plans. Schedule your evaluation now.
Frequently Asked Questions
Is a home sleep apnea test as accurate as an in-lab study?
For detecting moderate to severe obstructive sleep apnea, home tests are considered a reliable option. They may slightly underestimate severity compared to in-lab studies because they do not measure brain waves to determine exact sleep time, but they provide meaningful and actionable data for most people.
Do I need a prescription for a home sleep test?
Yes. Home sleep apnea tests are classified as medical diagnostic tools and require a prescription from a healthcare provider. SLIIIP offers options that include obtaining a prescription through a telemedicine consultation as part of the process.
How long does the test take?
The actual test is conducted during a single night of sleep. The entire process, from ordering to receiving results, typically takes one to two weeks depending on the provider.
What does a home sleep test measure?
Most home tests measure airflow, blood oxygen saturation, heart rate, breathing effort, and often body position and snoring. Some advanced devices also measure peripheral arterial tone and chest motion.
Can I use the bathroom during the test?
Yes. You can get up during the night. The device uses movement sensors to detect periods of activity, and that data is accounted for in the analysis.
What if the test does not work?
If sensors become dislodged or the device malfunctions, the provider may offer a free retest or recommend an in-lab study. The failure rate for home tests is relatively low, typically around 7 to 8 percent.
Does insurance cover home sleep tests?
Many insurance plans do cover home sleep apnea testing. Coverage varies by plan, so it is a good idea to check with your insurance provider before ordering. SLIIIP provides guidance on insurance coverage for home sleep studies.
How much does a home sleep test cost without insurance?
Costs vary by provider and device, but home tests are generally a fraction of the cost of an in-lab polysomnography. SLIIIP offers transparent pricing on their shop page.
Can a home test detect central sleep apnea?
Some newer home testing devices can detect central sleep apnea, which involves the brain failing to signal the muscles to breathe rather than a physical airway obstruction. However, the primary design of most home tests is focused on obstructive sleep apnea.
What is the Apnea-Hypopnea Index?
The AHI measures the average number of apneas (complete breathing pauses) and hypopneas (significant reductions in breathing) per hour of sleep. It is the primary metric used to determine the presence and severity of sleep apnea.
Can I do a home sleep test if I have other health conditions?
Home tests are appropriate for many people, but those with significant heart, lung, or neurological conditions may be better served by an in-lab study. Discuss your full health history with your provider before deciding.
How soon will I get my results?
Results are typically available within a few days to a week after the device data is submitted for analysis. SLIIIP connects you with a sleep specialist who reviews the data and provides a detailed report.
What should I do if my test shows sleep apnea?
If sleep apnea is identified, your provider will recommend a personalized approach based on the severity and your individual circumstances. Options may include CPAP therapy, oral appliances, positional therapy, lifestyle modifications, or a combination.
What if my test comes back normal but I still feel tired?
If your home test does not indicate sleep apnea but you continue to experience poor sleep quality, your provider may recommend a more comprehensive in-lab sleep study or evaluation for other sleep-related conditions. Persistent fatigue despite adequate sleep time can have many possible explanations.
Do I need to sleep on my back during the test?
It is helpful to spend some time sleeping on both your back and your side during the test. Sleep apnea is often more pronounced in the supine (back-sleeping) position, and having data from both positions gives the specialist a more complete picture.
Can I take sleep medication the night of the test?
You should follow your usual routine, but it is best to avoid sedatives or sleep aids on the night of the test unless specifically instructed otherwise by your provider. These substances can affect muscle tone and breathing patterns, potentially influencing results.
How do I set up the device?
Most home sleep test devices come with step-by-step instructions and often include video tutorials. The setup typically takes about 10 to 15 minutes. If you need help, most providers offer phone or video support to walk you through the process.
What is the difference between Type 3 and Type 4 sleep tests?
Type 3 tests use a greater number of sensors and measure more variables, including airflow, breathing effort, oxygen levels, heart rate, and body position. Type 4 tests are simpler and may only measure one or two variables, like oxygen levels. Most home sleep apnea tests used clinically today are Type 3.
Can children do home sleep tests?
Home sleep tests are generally designed for adults. Children suspected of having sleep apnea are usually evaluated with an in-lab polysomnography, which provides the more comprehensive monitoring appropriate for pediatric assessments. If you are concerned about sleep apnea in your child, SLIIIP has resources to help you take the first step.
Will a home sleep test diagnose other sleep disorders?
No. Home sleep tests are specifically designed to detect obstructive sleep apnea and, in some cases, central sleep apnea. They do not diagnose other conditions such as narcolepsy, restless leg syndrome, or other non-breathing sleep disorders. An in-lab sleep study is needed for those evaluations.
How often should I be tested for sleep apnea?
If you have been previously evaluated and your symptoms change significantly, such as notable weight gain, increased snoring, or worsening fatigue, it may be worth discussing a follow-up sleep study with your provider.
Latest posts
-
Can Sleep Apnea Cause Dry Mouth?
Sleep apnea causes dry mouth symptoms in many adults because unstable breathing during sleep often forces the body to rely on mouth breathing. Dr. Avinesh Bhar at SLIIIP.com provides virtual…
-
Why Do I Need to Pee So Much at Night? The Sleep Apnea Connection
Waking up repeatedly during the night to urinate can completely destroy sleep quality according to Dr. Avinesh Bhar. Many people assume this problem is simply part of aging, drinking too…
-
How Much Melatonin Should I Take? A Sleep Doctor’s Honest Guide
Most people get the dose of melatonin wrong on their very first try, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, says the answer to how much melatonin should…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

