👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Starting CPAP Therapy: A Complete Guide for New Users
So you have been thinking of starting CPAP Therapy. The device has arrived. The mask is in your hands. And you have no idea what to expect from the first night. That moment, somewhere between hopeful and overwhelmed, is where nearly every new CPAP user begins. Read Dr. Avinesh Bhar’ s guide to give yourself the best possible start: what the first nights feel like, how to manage the most common challenges, how to read your therapy data, and what the evidence says about sticking with it.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
Why the First Two Weeks Are the Most Important
Research on CPAP adherence consistently identifies the first two weeks of therapy as the period that most strongly predicts long-term use. Users who persist through the initial adjustment phase and use CPAP consistently in the early weeks are substantially more likely to still be using it one year later. Users who abandon therapy in the first two weeks, typically due to discomfort or frustration, rarely return to it.
This means the decisions you make and the support you access in the first fourteen nights matter more than almost anything else. Understanding what is normal, what is fixable, and what warrants a call to your provider can make the difference between a two-week experiment and a lasting habit.
The first night will almost certainly feel strange. That is expected. The sensation of wearing a mask, feeling pressurized air against your face, and hearing the soft white noise of the device is unfamiliar. Your brain, which has never experienced this before, may resist sleep for longer than usual. This is not a sign that CPAP is not working for you. It is a sign that your nervous system is encountering something new, and that it will need a few nights to habituate.
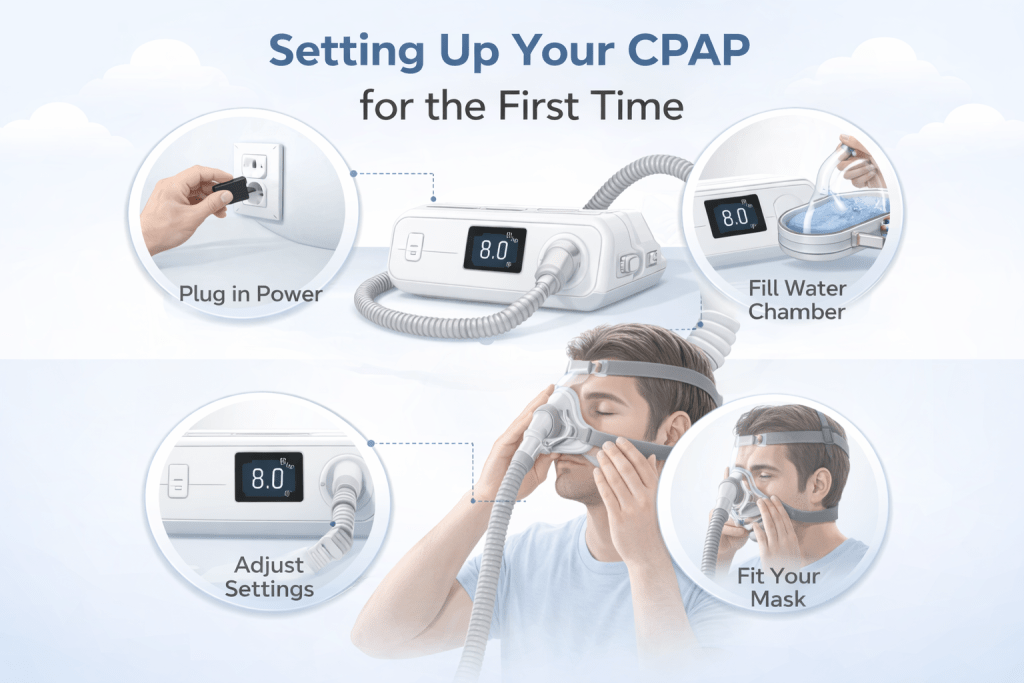
Setting Up Your CPAP for the First Time
Before your first night, take time to set up and familiarize yourself with the device in a relaxed setting. Sitting on the couch with the machine running and the mask on while watching television is one of the most frequently recommended acclimatization strategies, and there is a good reason for it. Experiencing the airflow while you are alert and unstressed reduces the novelty of the sensation and makes the transition to sleep easier.
Confirm your mask fit while you are sitting up and while you are lying in your normal sleep position. Masks fit differently in these two positions, and many fit-related issues only appear when you are horizontal. The headgear should be snug enough to maintain a seal but not so tight that it leaves significant marks or feels uncomfortable. A small amount of leak at the edges is acceptable. A sustained strong airflow escaping from the mask, particularly toward your eyes, indicates the seal needs adjustment.
Place the machine at roughly the same height as your sleeping surface if possible. This reduces the pull on the tubing during the night and minimizes the likelihood of the tube dragging the mask out of position when you roll over.
Your CPAP prescription specifies your pressure setting or auto-adjusting range. Do not adjust these settings yourself without guidance from your prescribing provider. The settings were determined based on your diagnostic results and are calibrated to your breathing patterns. Changing them without clinical direction can affect therapy effectiveness.
What the First Few Nights Feel Like
Most new CPAP users report a predictable sequence of experiences across the first week.
Night one to two: High awareness, variable sleep. The mask is very present in your consciousness. Falling asleep takes longer than normal. You may wake more frequently than usual. Some people remove the mask in the early hours of the morning without fully waking, a phenomenon called unconscious mask removal that is extremely common in new users.
Night three to five: Beginning habituation. The mask starts to feel less intrusive. Sleep onset time typically shortens. You may still wake once or twice but find it easier to settle again with the mask on.
Night six to fourteen: The critical threshold. Most users who make it to the second week are beginning to experience the benefits of therapy, often for the first time. Waking feeling more rested than before, reduced morning headaches, and more stable energy through the day are commonly reported early markers. These early improvements are powerful motivators for continued use.
If you are finding that you simply cannot sleep with the mask on in the first few nights, try the ramp feature on your CPAP machine if it has one. Ramp mode starts the device at a very low pressure and gradually increases to your prescribed setting over a period of ten to forty-five minutes. Many users find that falling asleep during the low-pressure ramp period and having the pressure increase only once they are already asleep makes the initial adjustment considerably easier.
The Most Common Early Challenges and How to Address Them
Mask Leaks and Air Escaping Around the Seal
This is the single most common issue new CPAP users encounter. Air escaping from around the mask cushion reduces the effective pressure delivered to your airway and can cause dry eyes, wind noise that disrupts sleep, and a rising AHI in your therapy data.
The most frequent causes are a cushion that is the wrong size, headgear that is too loose, or a mask style that does not suit your facial anatomy. Start by checking cushion size, which is separate from the mask frame size in most products, and experimenting with headgear tension. If leaks persist despite these adjustments, the mask style may not be the right fit for your face. Contacting your provider to try a different mask is the appropriate next step rather than continuing with a persistently leaking mask.
Dry Mouth
Waking with a dry, parched mouth is a very common early CPAP complaint. The most frequent cause is mouth breathing during sleep, which allows pressurized air to exit through the open mouth rather than being directed through the airway. If you are using a nasal or nasal pillow mask, adding a chin strap to encourage the jaw to stay closed during sleep often resolves this. If mouth breathing is habitual and the chin strap does not help sufficiently, switching to a full face mask is worth discussing with your provider.
Dry mouth can also occur with full face masks if the humidifier setting is too low. Increasing humidifier output generally helps. The experience of cotton mouth with CPAP is very common and very solvable, as explored in detail in the guide to dry mouth and CPAP.
Bloating and Air Swallowing
Some new CPAP users notice abdominal bloating or flatulence in the first weeks of therapy, caused by swallowing small amounts of pressurized air (aerophagia) rather than breathing it. This is more common at higher prescribed pressures and typically improves as you adjust to therapy. Sleeping with the head of the bed slightly elevated can help, as can ensuring your mask does not leak at the corners of your mouth if you are using a full face mask. More information is available in the guide to managing bloating and flatulence on CPAP.
Feeling Claustrophobic or Anxious
For some people, especially those who have never worn any kind of face covering during sleep, the sensation of a mask creates anxiety that makes sleep difficult. The most effective approach is gradual desensitization: wearing the mask for short periods while awake and comfortable before attempting to sleep in it. Nasal pillow masks, which cover the least surface area of any mask type, are often the best starting point for users who experience claustrophobia. The broader experience of struggling with CPAP in the early weeks is covered in the guide for people not loving their CPAP, which addresses the most common reasons early users want to give up.
Difficulty Breathing Out Against the Pressure
Some users find it physically difficult to breathe out against the continuous positive pressure. Most CPAP machines have an expiratory pressure relief (EPR or C-Flex) feature that reduces pressure slightly during the exhalation phase to make breathing more comfortable. If yours is not already activated, checking with your provider about enabling this feature is worth doing. It does not affect the therapeutic pressure during inhalation.
Reading Your Therapy Data Each Morning
Your CPAP machine records detailed data about every night of therapy. Reviewing this data, even briefly, each morning helps you identify problems early and have more productive conversations with your provider at follow-up appointments.
The key metrics to track are usage hours (aim for your full sleep duration every night), your AHI score (below 5 is the standard target, with many providers aiming for below 2), and your leak rate (check whether the device has flagged elevated unintentional leakage). A detailed explanation of each metric and what the numbers mean is available in the AHI score and CPAP data guide.
A single night with a higher AHI or a leak flag is not cause for concern. A consistent pattern over multiple nights is. If your AHI remains consistently above 10 after the first two weeks despite using the device, or if leak alerts appear every night, contact your provider to review your data and consider whether a pressure adjustment or mask change is warranted.
CPAP Supplies and Maintenance
A clean mask is a comfortable mask and a better-sealing mask. The following maintenance routine is simple but important.
Rinse your mask cushion daily with warm water. Wash it with mild, fragrance-free soap once a week. Rinse thoroughly and allow all components to air dry fully before the next use. Avoid machine washing headgear, which degrades the elastic. Do not use alcohol-based cleaners, bleach, or scented products on silicone components.
CPAP supplies have scheduled replacement intervals. Mask cushions typically last one to three months. The mask frame lasts approximately six months. Tubing and filters have their own replacement schedules.
Most insurance plans cover regular resupply of CPAP components. Setting up an automatic resupply schedule through your provider or DME supplier ensures you always have fresh components without having to track replacement dates manually. The CPAP supplies guide covers replacement schedules and insurance resupply options in detail.
If you need to take a break from CPAP due to illness, it is worth knowing what the guidance is on pausing therapy without losing the benefits you have built. The guide to taking a break from CPAP covers what to expect and when to resume.

SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
How Long Until You Feel Better?
There is no universal timeline, but most consistent CPAP users report noticing meaningful improvements within the first two to four weeks of regular nightly use. Common early positive changes include waking with more energy, fewer morning headaches, reduced daytime sleepiness, and feedback from a partner that snoring has reduced or stopped.
Some users report feeling dramatically better within the first few nights. Others take longer to notice changes, particularly if their sleep-disordered breathing was long-standing and their body has been operating in a state of chronic sleep fragmentation for years. Patience through the first month is consistently the most important factor separating users who benefit from therapy from those who give up before the benefits have time to manifest.
If you are three to four weeks into consistent CPAP use and not noticing any improvement in your daytime symptoms, contact your provider to review your data. A pressure adjustment, mask change, or further clinical evaluation may be warranted.
Not yet started on CPAP? Your first step is a home sleep test.
Complete a home sleep apnea test from your own bed. Results reviewed by a board-certified physician. Prescription issued when appropriate.
Getting CPAP Support Through SLIIIP
SLIIIP provides CPAP therapy through a fully online platform, from the initial home sleep test and prescription through device delivery and ongoing clinical support. Sleep medicine physician Dr. Avinesh Bhar and the wider SLIIIP clinical team are available to review your therapy data remotely, adjust your prescription if needed, and support you through the adjustment period without requiring in-person visits.
If you are already a SLIIIP patient and experiencing challenges in the early weeks of therapy, reaching out through the patient portal is the fastest route to getting your specific situation reviewed and addressed. The CPAP service page and the best CPAP mask guide are also useful starting points for new users navigating equipment decisions.
Already on CPAP and struggling?
SLIIIP’s clinical team can review your therapy data remotely and help identify what is making therapy difficult. No in-person visit required.
Frequently Asked Questions for New CPAP Users
How long does it take to get used to CPAP?
Most users begin to feel the benefits of therapy within two to four weeks of consistent nightly use. The initial adjustment period, where the mask and airflow feel unfamiliar, typically shortens significantly within the first week. Full habituation, where the device feels like a normal part of your sleep routine, often takes four to eight weeks.
What should I do on my first night with CPAP?
Set up the device in a familiar, relaxed environment. Practice wearing the mask while awake before trying to sleep in it. Use the ramp feature if your machine has one. Expect the first night to take longer to fall asleep than normal. Do not be discouraged if you wake during the night or remove the mask unconsciously. These are normal first-night experiences.
Is it normal to feel worse before feeling better on CPAP?
Some users report feeling more tired in the first few nights as their bodies adjust to a new sleep experience. This is not unusual and generally resolves within the first week. It does not indicate that therapy is wrong for you.
What is a good AHI score on CPAP?
Most sleep medicine guidelines consider a residual AHI below 5 events per hour to be within the normal range during therapy, with many providers targeting below 2. If your AHI is consistently above 10 despite using the device, contact your provider to review the data.
How tight should my CPAP mask be?
The mask headgear should be snug enough to maintain a seal when you are lying in your normal sleep position, but not so tight that it causes discomfort, skin indentation, or restricted circulation. A slight intentional seal adjustment that reduces leaks without over-tightening is the goal. If you consistently wake with red marks or skin impressions, the mask is too tight.
Why does my CPAP give me a dry mouth?
Dry mouth on CPAP is almost always caused by mouth breathing, which allows pressurized air to escape through the open mouth. A chin strap with a nasal or nasal pillow mask, or switching to a full face mask, resolves this in most cases. Low humidifier settings can also contribute to dryness and are worth adjusting.
Can I use CPAP if I have a cold or nasal congestion?
CPAP can typically still be used during a cold, though nasal congestion may make it more uncomfortable, particularly with nasal-only mask styles. Nasal saline rinse before bed, humidifier adjustments, and temporarily switching to a full face mask if you normally use a nasal mask can all help. Guidance on managing CPAP use while unwell is covered in the dedicated article on common CPAP challenges.
How many hours of CPAP use do I need per night?
Insurance compliance typically requires a minimum of four hours per night on 70 percent or more of nights over a 30-day period. For optimal clinical benefit, most providers recommend using CPAP for the full duration of your sleep every night.
Can I take a night off from CPAP?
Occasional missed nights do not erase the benefits of consistent use. However, the symptoms of sleep-disordered breathing typically return on nights CPAP is not used. Habitual skipping of therapy undermines the cumulative benefits. If you are avoiding CPAP regularly because of discomfort, identifying and addressing the specific cause is more productive than accepting frequent therapy gaps.
Why does my CPAP machine make noise?
A properly functioning CPAP machine produces a low, consistent hum that most users find easy to habituate to or even soothing. Increased noise often indicates air leaking from the mask seal or tubing connection. Checking all connection points and mask fit usually resolves unexpected noise. If the machine itself sounds different from normal, contact your provider.
Should I clean my CPAP mask every day?
Rinsing the mask cushion daily with warm water is recommended. A full wash with mild soap once a week helps prevent the buildup of oils, bacteria, and residue that can degrade the silicone and cause skin irritation. Regular cleaning also helps maintain the integrity of the seal.
How do I know if my CPAP pressure needs adjusting?
Signs that your pressure may need adjustment include a consistently elevated residual AHI, persistent difficulty exhaling comfortably against the pressure, or continued symptoms such as fatigue and morning headaches despite regular use. All of these are reasons to contact your prescribing provider rather than adjusting settings yourself.
Can CPAP therapy be used by people who sleep on their stomach?
Stomach sleeping with CPAP is challenging because most masks are displaced when the face is pressed directly into a pillow. Nasal pillow masks offer the most minimal profile and are the most viable option for stomach sleepers. Some users modify their pillow setup to create a cutout for the mask. If stomach sleeping is your only comfortable position and masks are consistently displaced, discussing this with your provider is worthwhile.
What is the ramp feature on a CPAP machine?
The ramp feature starts your CPAP at a low pressure setting and gradually increases it to your prescribed level over a set time period, typically ten to forty-five minutes. This allows you to fall asleep before full therapy pressure is reached, which many new users find more comfortable than full pressure from the moment the machine is switched on.
How often do I need to replace CPAP supplies?
Replacement schedules vary by component. Mask cushions are typically replaced every one to three months. The full mask frame every six months. Tubing and filters have their own intervals. Most insurance plans cover regular supply resupply, and most DME providers offer automated resupply programs to manage this.
What do I do if CPAP therapy is not improving my symptoms?
After four weeks of consistent therapy without improvement in daytime symptoms, contact your prescribing provider to review your therapy data. A pressure adjustment, mask change, or further clinical evaluation may be needed to optimize your therapy.
Can I travel with my CPAP machine?
Yes. CPAP machines are recognized as medical devices and are permitted in aircraft cabins without counting against carry-on limits on most airlines. Travel-size CPAP machines and battery power options make overnight travel and off-grid use more manageable. SLIIIP can advise on travel CPAP options appropriate for your prescription.
Is it normal to swallow air on CPAP?
Aerophagia, the swallowing of small amounts of pressurized air, is a known side effect of CPAP therapy, particularly at higher pressures. It can cause bloating, belching, and flatulence. It typically improves with time and can often be reduced by sleeping with the head of the bed elevated, ensuring the mask does not leak, and in some cases through a pressure or therapy mode adjustment.
What is the difference between CPAP and APAP?
CPAP (continuous positive airway pressure) delivers a fixed, constant pressure throughout the night. APAP (auto-adjusting positive airway pressure) uses a variable pressure that responds to your actual breathing patterns, delivering higher pressure when needed and lower pressure when breathing is stable. Many new users are prescribed APAP for its comfort flexibility. Your prescription will specify which mode you are on.
Thank you for reading this article.
Latest posts
-
What Caffeine Does to Deep Sleep: How Caffeine and Deep Sleep Quietly Compete
Caffeine and deep sleep are quietly at odds. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. You can fall asleep at…
-
Caffeine Metabolism: Fast vs Slow Metabolizers and Why the Same Cup Hits Differently
Caffeine metabolism is highly variable, according to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. Two people can drink the exact same coffee…
-
The 6 Hour Rule: What the Research Actually Says About Caffeine Cutoff Times
The 6 hour rule is frequently questioned. According to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, many individuals experience symptoms without clear awareness. You may have heard that you…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.


