👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Why Do I Feel Depressed and Tired All the Time?
If you find yourself dragging through every day, wondering “Why do you I feel depressed and tired all the time?” Dr. Avinesh Bhar has heard this daily from patients who suffer from a sleep disorder.
Many people assume depression causes their fatigue, or that fatigue is causing their low mood. The reality is often more complex. Depression and tiredness feed into each other in a cycle that can be difficult to break, and in many cases, there is an underlying factor making both worse: disrupted sleep.
This article explores why depression and fatigue are so tightly connected, what might be driving both symptoms, and what you can do to start feeling better.
Understanding the Depression-Fatigue Connection
Depression is far more than persistent sadness. It is a medical condition that affects your brain chemistry, your hormones, your energy levels, and your physical health. Research shows that over 90% of people with depression experience significant fatigue. For many, exhaustion is actually the most noticeable symptom, sometimes appearing before mood changes become obvious.
Depression disrupts the neurotransmitters in your brain that regulate alertness, motivation, and energy, particularly serotonin, norepinephrine, and dopamine. When these chemical messengers are out of balance, your body’s ability to feel awake, engaged, and energized is compromised at a fundamental biological level.

Why Does Depression Make You So Tired?
Disrupted Sleep Architecture
Depression changes the structure of your sleep. People with depression tend to spend more time in lighter sleep stages and less time in the deep, restorative stages that help your body and brain recover. Sleep becomes more fragmented, and even when you sleep for a long time, the sleep itself is not doing its job.
Dr. Avinesh Bhar explains how sleep gets affected and then your mood when you have a sleep disorder.
Neurotransmitter Imbalances
The same brain chemicals involved in depression, such as serotonin and norepinephrine, also regulate your energy and wakefulness. When these systems are disrupted, fatigue is a direct consequence, not just a side effect of feeling sad.
Chronic Stress and Cortisol
Depression is closely linked to chronic stress, which keeps your body in a prolonged “fight or flight” state. Over time, elevated cortisol levels deplete your energy reserves, leaving you feeling exhausted even when you have not been physically active.
Appetite and Nutrition Changes
Depression commonly disrupts eating patterns. Some people eat less, missing essential nutrients. Others turn to high-sugar, high-fat comfort foods that cause energy crashes. Both patterns contribute to the heavy, drained feeling that accompanies depression.
Medication Side Effects
Some antidepressant medications, particularly SSRIs, can cause fatigue as a side effect. This creates a frustrating paradox where the treatment for depression may actually worsen the tiredness. If you suspect your medication is contributing to your fatigue, discuss this with your prescribing provider. Adjustments or alternatives may help.
The Hidden Link: Sleep Disorders and Depression
Important: Research has found that depression is common in people with obstructive sleep apnea, and that the severity of depression often correlates with the severity of the sleep apnea. Treating the sleep disorder frequently improves depression symptoms, sometimes dramatically. |
Here is something that many people do not realize: undiagnosed sleep disorders, particularly obstructive sleep apnea (OSA), can mimic or worsen depression. When your breathing is repeatedly interrupted during sleep, your brain is deprived of oxygen, your sleep is fragmented, and your body never fully recovers. The result is chronic fatigue, irritability, difficulty concentrating, and a pervasive low mood, all symptoms that overlap with clinical depression.
Studies show that up to 50% of people with obstructive sleep apnea also meet the criteria for depression.
Signs That a Sleep Disorder May Be Contributing to Your Depression
- You feel exhausted no matter how much you sleep
- Your partner has noticed loud snoring, gasping, or pauses in your breathing
- You wake up with headaches, dry mouth, or a sore throat
- You have difficulty concentrating or experience brain fog
- Antidepressant medication has not fully resolved your symptoms
- You feel more irritable than sad
What You Can Do: Steps Toward Feeling Better
Talk to Your Doctor About a Sleep Evaluation
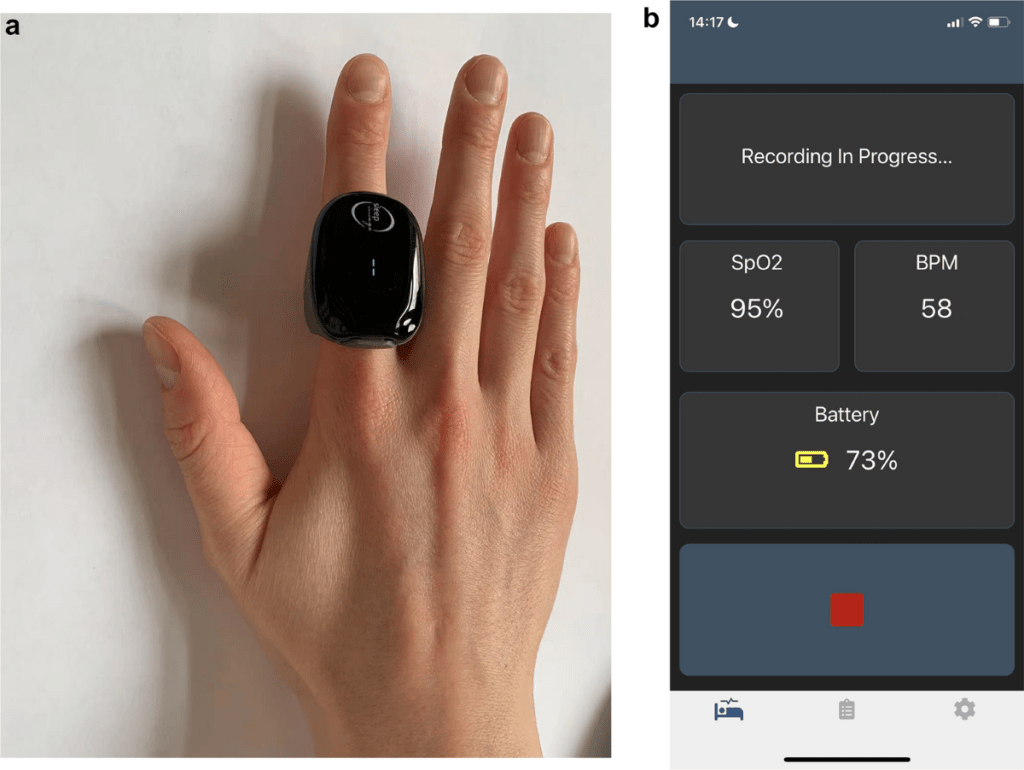
If you have been dealing with depression and fatigue, ask your healthcare provider about the possibility of a sleep disorder. A home sleep apnea test is a simple, convenient way to screen for conditions like obstructive sleep apnea. Telemedicine services like SLIIIP make it possible to consult with a board-certified sleep specialist from home and receive a home sleep test without the delays of traditional referrals.
Prioritize Sleep Hygiene
Maintaining a consistent sleep and wake schedule, keeping your bedroom cool and dark, limiting screen time before bed, and avoiding caffeine and alcohol in the evening can all improve sleep quality. While these steps alone may not resolve a sleep disorder, they create a foundation for better rest.
Stay Physically Active
Exercise is one of the most effective interventions for both depression and fatigue. Even gentle activity like a daily walk can boost neurotransmitter levels, reduce stress hormones, and improve sleep quality over time.
Seek Professional Support for Your Mental Health
Cognitive behavioral therapy (CBT), particularly CBT for insomnia (CBT-I), has strong evidence for improving both depression and sleep. A qualified therapist can help you break the cycle of negative thoughts, poor sleep, and low energy.
Treatment for Sleep Apnea: CPAP and Beyond
If a sleep study reveals obstructive sleep apnea, treatment can be life-changing, not just for your sleep, but for your mood and energy. CPAP therapy is the most commonly prescribed treatment, using gentle air pressure to keep your airway open throughout the night. For patients who find CPAP difficult to use, oral appliance therapy offers an effective, comfortable alternative.
Oral Appliance Therapy: What Patients Want to Know
Oral appliances, also called mandibular advancement devices, are custom-fitted dental devices worn during sleep. They gently reposition the lower jaw forward to prevent airway collapse.

They are quiet, portable, and for many patients, easier to use consistently than CPAP. Below, dentists who specialize in dental sleep medicine answer frequently asked questions:
|
Q: I have been diagnosed with both depression but I don’t think I have sleep apnea.
|
|
Dr. Keya Patel I gently shift the conversation to what they care about most: showing up fully for their family, having energy that lasts through the day, protecting their brain and heart long-term. Once we connect those dots, they’re usually more open to learning. The home sleep test gives answers. It’s not about putting a label on someone—it’s about seeing clearly and taking action early. When the conversation shifts to values instead of symptoms, people start to realize: maybe it’s worth checking.” |
|
Q: Is an oral appliance more comfortable than CPAP? |
|
Dr. Derek M. Cornetta, DDS, FAGD https://www.woodsidedentalcare.com
|
|
Q: What to Expect During the Oral Appliance Fitting Process |
|
DDS, FAGD, D.ABDSM https://www.summerland-dental.com/ Once determined to be a suitable candidate for an oral appliance, you’ll move on to the fitting appointment. During this visit, impressions of your teeth will be taken. At Summerland Dental, we use a state-of-the-art oral scanner for our impressions to digitally create custom-fit models. This process is painless and usually takes about 15-30 minutes. Following the digital impressions, the dentist will also take bite records to establish your jaw’s current position. These records will be sent to a specialized sleep dental laboratory, where the oral appliance is constructed. The device is designed to fit comfortably in your mouth, helping to maintain an open airway during sleep. Once your custom appliance is ready, you will return for a fitting appointment. This visit is crucial, as the dentist will ensure that the appliance fits properly and make any necessary adjustments for optimal comfort and function. It might take a few nights to adjust, so it’s essential to communicate any discomfort or issues during this period. Periodic follow-ups will also be scheduled to assess the appliance’s effectiveness and make adjustments if necessary. Once the appliance has be optimized, a new home sleep test will be done to compare to your original one to see how much improvement has occurred.” |
Frequently Asked Questions
Can sleep apnea cause depression?
Yes. Research strongly supports the connection between obstructive sleep apnea and depression. The chronic sleep fragmentation and oxygen deprivation caused by OSA can directly affect mood-regulating brain chemicals. Treating OSA has been shown to significantly improve depressive symptoms in many patients.
Why am I tired all the time even though I am not sad?
Depression does not always present as sadness. Many people experience depression primarily through physical symptoms like fatigue, difficulty concentrating, and loss of interest in activities. Additionally, conditions like sleep apnea, anemia, thyroid disorders, and vitamin deficiencies can cause chronic tiredness independent of mood changes.
Should I see a sleep specialist or a therapist first?
If your fatigue is a prominent symptom, starting with a sleep evaluation can help identify or rule out a sleep disorder that may be contributing to both your tiredness and your mood. Ideally, addressing both sleep and mental health simultaneously provides the best outcomes.
Latest posts
-
Best Alternatives to Sleeping Pills for Anxiety
The best alternatives to sleeping pills for anxiety are reshaping how modern sleep medicine treats restless minds, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, has watched the shift…
-
Top Natural Sleep Aids: What Actually Works for Better Rest
Top natural sleep aids have quietly taken over bedside tables across the country, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, sees the same pattern every week: people stack…
-
Best Treatments for Insomnia Caused by Anxiety
The best treatments for insomnia caused by anxiety hit both sides of the loop at once, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, has watched this two-front approach…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.

