👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

Dental Device for Sleep Apnea: Cost and Coverage
When people first learn that a small custom-fitted dental device may be an alternative to a CPAP machine for managing sleep-disordered breathing, the first question is almost always the same: how much does it cost? Dr. Avinesh Bhar explains the best dental device for sleep apnea in this guide.
If you have been exploring oral appliance therapy as a potential fit for your situation, understanding the financial picture before you begin the process will save you from surprises and help you plan accordingly.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
What Is a Dental Device for Sleep Apnea?
A dental device for sleep apnea is a custom-fabricated oral appliance worn during sleep. The most common type is a mandibular advancement device (MAD), sometimes also called a mandibular repositioning device or simply an oral appliance. The device fits over the upper and lower teeth and holds the lower jaw in a slightly forward position while you sleep.
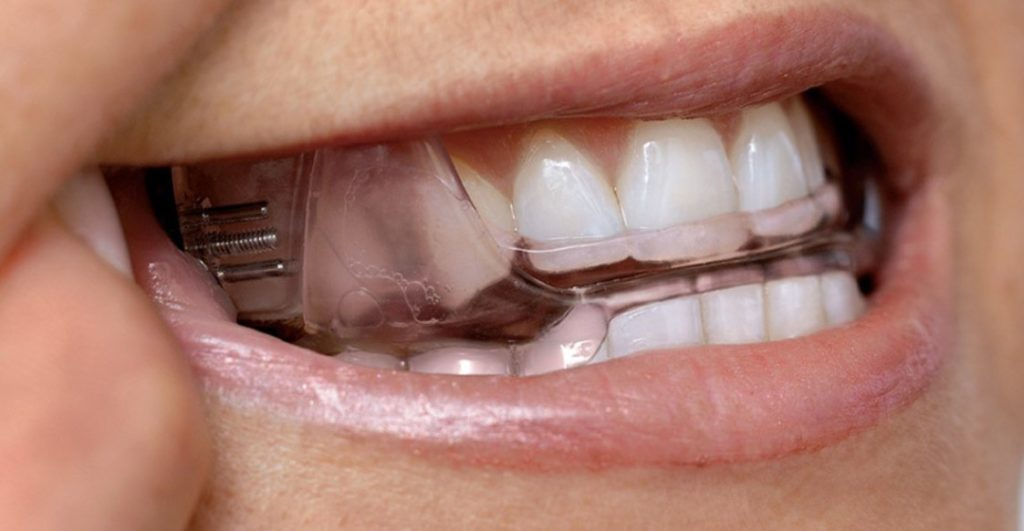
This forward jaw positioning helps maintain a more open space in the upper airway, reducing the likelihood that soft tissue at the back of the throat will collapse and restrict airflow. The degree of advancement is adjustable and is gradually calibrated over several follow-up visits to find the position that delivers the best balance of therapeutic effect and physical comfort.
Oral appliances are prescribed medical devices, not over-the-counter products. They require a diagnosis from a sleep study or home sleep test and a valid prescription from a licensed physician. The fabrication is performed by a dental laboratory from precise impressions or digital scans of your teeth. This precision is what distinguishes a genuine therapeutic device from a generic boil-and-bite mouthguard available in a pharmacy.
For a more detailed introduction to how oral appliances work and the full range of options available, the complete guide to oral appliance therapy for sleep apnea covers the clinical context in depth.
How Much Does a Dental Device for Sleep Apnea Cost Without Insurance?
The out-of-pocket cost of a custom oral appliance for sleep apnea, when paying without insurance, typically falls between $1,800 and $3,500. This range encompasses the full process: the initial consultation, the dental impressions or digital scans, the laboratory fabrication of the device, and the follow-up titration appointments where the jaw advancement is adjusted to its optimal setting.
Several factors influence where a specific case lands within this range.
Device model and laboratory. Different oral appliance designs, such as the SomnoDent, the Herbst appliance, or the myTAP, vary in fabrication complexity and material cost. A two-piece titratable device with a precision adjustment mechanism will generally cost more to fabricate than a simpler single-piece design.
The dental provider’s fees. Geographic location, provider experience in sleep-related dentistry, and the clinic’s overhead all contribute to the consultation and follow-up fees charged alongside the device cost itself. Dental providers in major metropolitan areas typically charge more than those in smaller markets.
Number of follow-up appointments needed. The titration process, where advancement is incrementally increased to optimize the therapeutic position, varies in how many visits it requires. More complex cases requiring multiple adjustments before finding a stable position will naturally cost more in total.
Whether a diagnostic sleep study is included. If you have not yet had a qualifying sleep study, that cost is separate from the device itself. A home sleep test, which is generally less expensive than an in-lab study, typically ranges from $200 to $500 without insurance, though many plans cover it fully or partially.

It is worth noting that over-the-counter boil-and-bite mouthguards marketed for snoring are sold for $20 to $100 and are categorically different from prescription oral appliances. They are not fabricated to your dental anatomy, they do not deliver controlled mandibular advancement, they cannot be titrated, and they are generally not considered equivalent for managing sleep-disordered breathing. If you are weighing the cost of a custom device, comparing it to an OTC mouthguard is not an accurate comparison.
Does Insurance Cover a Dental Device for Sleep Apnea?
This is the most consequential question for most people, and the answer is: yes, frequently, with specific conditions. Most major commercial health insurance plans categorize custom oral appliances for sleep apnea as durable medical equipment (DME), meaning they fall under the medical insurance benefit rather than the dental insurance benefit. This is an important distinction that many patients miss. Submitting a claim to your dental insurer for an oral appliance will almost always be denied. The claim belongs with your medical insurer.
For coverage to apply, the following conditions are typically required.
A qualifying sleep study or home sleep test. Your insurer will require documentation that a sleep-disordered breathing condition has been formally identified through a recognized diagnostic study. A home sleep test conducted through an approved provider and reviewed by a board-certified sleep physician generally satisfies this requirement.
A valid physician prescription. A prescription for oral appliance therapy issued by a licensed sleep medicine physician. The prescription must document the diagnosis, the prescribed therapy type, and the medical necessity.
A participating DME provider or dental provider. Insurers typically require that the device be provided by a provider or dental practice that is enrolled in their network as a durable medical equipment supplier. Using an out-of-network provider may result in higher cost-sharing or denial of the claim.
Prior authorization. Many plans require prior authorization before approving an oral appliance. This means your provider must submit clinical documentation to the insurer for review and approval before the device is fabricated. Working with a provider who manages this process as part of their standard workflow, as SLIIIP does, simplifies this step considerably.
When all these conditions are met, cost-sharing through insurance typically mirrors the plan’s DME benefit. Depending on the specific plan, this might mean paying a fixed copay, meeting a deductible, or paying a percentage of the approved cost up to an out-of-pocket maximum. In some cases, the device is covered at or near 100 percent after the deductible is met. In others, the patient may be responsible for 20 to 30 percent of the approved cost.
For a full breakdown of how medical insurance applies to sleep apnea equipment in general, the CPAP and sleep apnea equipment insurance coverage guide covers the major plan types and common coverage scenarios in detail.

Not yet diagnosed? Your home sleep test may be fully covered.
A home sleep apnea test is typically the first step toward getting a prescription for an oral appliance. Many insurance plans cover the test in full. Complete yours from home, reviewed by a board-certified physician.
Medicare and Medicaid Coverage
Medicare Part B may cover oral appliances for sleep apnea under its durable medical equipment benefit when the following conditions are met: the device is prescribed by a physician, provided by a Medicare-enrolled DME supplier, and supported by documentation from a qualifying sleep study demonstrating sleep-disordered breathing of the relevant severity.
Medicare coverage for oral appliances has historically been less straightforward than CPAP coverage, and the specific criteria, approved device codes, and participating supplier requirements are subject to periodic updates. Contacting your Medicare plan administrator or a Medicare DME specialist directly is the most reliable way to confirm current coverage terms for your specific situation.
Medicaid coverage for oral appliances varies by state, as Medicaid programs are administered at the state level with different DME formularies and prior authorization requirements. Checking with your state Medicaid office or a participating dental provider who works with Medicaid patients is the appropriate first step.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
HSA and FSA Eligibility
Custom oral appliances for sleep apnea are generally eligible medical expenses under both Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA). Because they are prescription medical devices prescribed by a licensed physician for a diagnosed condition, they typically qualify as reimbursable out-of-pocket medical costs under IRS guidelines governing these accounts.
If you are paying any portion of the oral appliance cost out of pocket, using pre-tax HSA or FSA funds to cover that cost reduces your effective out-of-pocket expense by the amount of your marginal tax rate. Confirming the specific eligibility of the device and the associated dental fees with your HSA or FSA plan administrator before submitting reimbursement is advisable.
At SLIIIP we also accept these insurances and Medicare.

Dental Device vs. CPAP: A Cost Comparison
For people evaluating whether to pursue oral appliance therapy or CPAP therapy, cost is often one of several factors. Understanding how the two compare financially helps frame the decision more clearly.
A CPAP machine typically costs between $500 and $1,500 for a standard home unit, with premium models reaching $2,000 or more. When obtained through insurance with a qualifying prescription, most CPAP machines are covered under the DME benefit, often with a monthly rental structure that leads to ownership after a standard rental period, typically 13 months. Masks, tubing, and filters require regular replacement, adding an ongoing supply cost that most insurance plans also cover on a resupply schedule.
A custom oral appliance, as noted, typically costs between $1,800 and $3,500 without insurance, with a one-time fabrication cost and periodic follow-up appointments. There are no ongoing consumable supplies comparable to CPAP masks and filters. The device is replaced every three to five years when it shows wear or when dental changes require a new fit.
Over a five-year period, the total cost of CPAP therapy, including supplies, is often comparable to or greater than the total cost of an oral appliance, particularly when insurance covers neither fully. The comparison shifts significantly when insurance is involved, as CPAP coverage tends to be more straightforward and more comprehensively covered by most plans. A side-by-side analysis of the two approaches from a clinical perspective is available in the oral appliance vs. CPAP comparison guide.
How to Get a Dental Device for Sleep Apnea Through SLIIIP
SLIIIP offers a streamlined pathway to oral appliance therapy that begins with a home sleep test and ends with a prescription issued by a board-certified sleep medicine physician. The process is designed to eliminate the unnecessary delays and administrative friction that often slow down access to sleep-disordered breathing management.
The first step is completing a home sleep test, which documents whether sleep-disordered breathing is present and, if so, its general severity. The test is conducted from home using a compact wrist sensor and is reviewed by a physician within a few business days. If the results support an oral appliance prescription, the prescription is issued and coordinated with a participating dental provider for device fabrication.
The entire process, from ordering a home sleep test to receiving a prescription, can be completed in as little as one to two weeks in most cases. SLIIIP’s clinical team, led by sleep medicine physician Dr. Avinesh Bhar, manages prior authorization submissions and works with your insurance plan to maximize coverage before the device is ordered.
For those specifically interested in the myTAP device, which is one of the available oral appliance options through SLIIIP’s platform, the myTAP oral appliance review covers its design, fit, and user experience in detail. For an overview of the full range of prescription oral appliances available, the guide to the top-rated oral appliances provides a comparative breakdown.
For those interested in the expedited OAT prescription pathway specifically, the fast OAT prescriptions page outlines how SLIIIP handles the process from start to finish.
What to Ask Before Committing to an Oral Appliance
Going into the process informed makes everything easier. The following questions are worth raising with your provider or insurer before beginning.
Is a prior authorization required by my insurance plan for an oral appliance? If yes, which diagnosis codes and clinical documentation will be needed? Which participating DME providers or dental practices does my plan recognize for this benefit? What is my deductible status and what will my estimated cost-sharing be after the approved cost? Is the home sleep test required to qualify for coverage, and is that test itself covered under my plan?

SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
Having clear answers to these questions before the device is ordered eliminates the risk of unexpected costs after the fact. A good sleep medicine provider will help you navigate these questions as part of the intake process.
Want to know what your plan covers before you commit?
Many insurance plans cover oral appliances for sleep apnea under their medical DME benefit. SLIIIP can help verify your benefits and manage prior authorization before any cost is incurred.
Verify Your Insurance Coverage
Oral Appliance Therapy: What the Research Suggests
The evidence base for oral appliance therapy has grown substantially over the past two decades. According to the American Academy of Sleep Medicine, custom oral appliances are a recognized therapeutic option for sleep-disordered breathing, particularly for individuals with mild to moderate presentations or for those who have not tolerated CPAP therapy.
Research generally shows that while CPAP tends to achieve a more complete reduction in AHI values under controlled conditions, oral appliances may produce comparable improvements in daytime function and quality of life in many users, partly because higher adherence rates offset the slightly lower per-night efficacy. In other words, a therapy that is worn consistently throughout the night tends to produce better real-world outcomes than a more potent therapy that is frequently discontinued or used inconsistently.
The clinical picture for any individual depends on the severity and pattern of their sleep-disordered breathing, their dental anatomy, and their lifestyle. A sleep medicine physician is best positioned to evaluate whether oral appliance therapy is a clinically appropriate option given your specific diagnostic results. For context on the full spectrum of oral appliance options and how they compare, the comprehensive oral appliance guide and the custom oral appliance vs. mouthguard comparison cover the key distinctions clearly.
Frequently Asked Questions About Dental Device for Sleep Apnea Cost and Coverage
How much does a dental device for sleep apnea cost?
The cost of a custom dental device for sleep apnea typically ranges from $1,800 to $3,500 without insurance. This range reflects the dental fitting process, custom fabrication, and follow-up adjustment appointments. Over-the-counter boil-and-bite mouthguards are not the same as a prescription oral appliance.
Does insurance cover a dental device for sleep apnea?
Many medical insurance plans, including major commercial plans and Medicare, cover custom oral appliances when prescribed by a licensed physician following a qualifying sleep study. Coverage requires documentation of a sleep apnea diagnosis, a valid prescription, and use of a participating DME provider. Dental insurance generally does not cover sleep apnea oral appliances.
What is a dental device for sleep apnea called?
A dental device for sleep apnea is most commonly called an oral appliance, a mandibular advancement device (MAD), or a mandibular repositioning device. The generic term oral appliance therapy (OAT) refers to the use of these devices as a category of sleep-disordered breathing management.
Who is a good candidate for a dental device for sleep apnea?
Oral appliances are commonly considered for people with mild to moderate sleep-disordered breathing who prefer an alternative to CPAP therapy, or for those who have not tolerated CPAP well. They are also used for frequent travelers who want a compact, non-electric therapy option.
Do I need a prescription for a dental device for sleep apnea?
Yes. A custom oral appliance for sleep apnea requires a prescription from a licensed physician, issued following a sleep study or home sleep apnea test. Over-the-counter mouthguards available without a prescription are different products and are not considered equivalent to a custom-fitted oral appliance.
How does a dental device for sleep apnea work?
A mandibular advancement device holds the lower jaw in a slightly forward position during sleep. This forward positioning helps maintain a more open airway by preventing the soft tissue at the back of the throat from collapsing. The device is custom-fabricated and adjusted over time to find the optimal jaw position.
Is a dental device as effective as CPAP for sleep apnea?
CPAP is generally considered the most well-studied approach for moderate to severe sleep-disordered breathing. For mild to moderate cases, research suggests custom oral appliances may achieve comparable outcomes. The best option for any individual depends on severity, anatomy, and personal preference. A sleep medicine physician can help determine which approach is appropriate.
Does Medicare cover a dental device for sleep apnea?
Medicare Part B may cover oral appliances under its DME benefit when prescribed by a physician and provided by a Medicare-enrolled DME supplier. Coverage requires a qualifying sleep study and documentation of medical necessity. Contacting your Medicare plan administrator is the best way to confirm current coverage terms.
How long does a dental device for sleep apnea last?
Most custom oral appliances are designed to last between three and five years with proper maintenance and regular use. Regular follow-up with your dental provider helps assess device condition and identify when replacement is needed.
What is the difference between a custom oral appliance and an over-the-counter mouthguard?
A custom oral appliance is fabricated from precise dental impressions, fitting your exact dentition and delivering a controlled degree of mandibular advancement. An OTC boil-and-bite mouthguard does not provide the same precision of fit or controlled jaw positioning. Custom appliances are significantly more effective and comfortable for managing sleep-disordered breathing.
Are there side effects of wearing a dental device for sleep apnea?
Common initial experiences include mild jaw soreness, tooth sensitivity, and increased salivation, particularly in the first few weeks of use. These often resolve with time. Long-term use has been associated with minor bite changes in some users. Regular dental monitoring is recommended.
Can I use a dental device for sleep apnea if I have dentures?
Traditional mandibular advancement devices rely on anchoring to natural teeth. Full denture wearers may not be suitable candidates for standard oral appliances. A dental provider familiar with sleep-disordered breathing management can advise on alternative options depending on the individual situation.
How is a dental device for sleep apnea fitted?
The fitting process typically involves dental impressions or a digital scan, used by a dental laboratory to fabricate a custom device. A titration process gradually increases jaw advancement over several follow-up visits to find the optimal therapeutic position.
How long does it take to get used to a dental device for sleep apnea?
Most users adapt to wearing an oral appliance within two to four weeks. Initial jaw soreness and device awareness during sleep are common in the first week and generally resolve with continued nightly use.
Can a dental device for sleep apnea be used for travel?
Yes. An oral appliance is small, lightweight, requires no electricity, and can be packed in carry-on luggage without any equipment restrictions. Many CPAP users choose an oral appliance specifically as a travel alternative.
What is the fastest way to get a dental device for sleep apnea?
The fastest pathway typically involves completing a home sleep test to obtain a diagnosis and prescription, then working with a telemedicine sleep clinic that offers an expedited oral appliance therapy pathway. SLIIIP offers a streamlined OAT prescription process for qualified patients.
Can I get a dental device for sleep apnea online?
The prescription can be obtained through a telemedicine sleep medicine provider following a home sleep test. The physical fabrication of the device still requires dental impressions or scans, coordinated through a participating dental provider.
Is a dental device for sleep apnea covered by HSA or FSA?
Custom oral appliances for sleep apnea are generally eligible for reimbursement under both Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA) as out-of-pocket medical costs. Confirming eligibility with your plan administrator before submitting reimbursement is advisable.
What does oral appliance therapy involve?
Oral appliance therapy (OAT) involves wearing a custom-fitted dental device during sleep that holds the lower jaw forward to help keep the upper airway open. Therapy includes an initial fitting, a titration period, and periodic follow-up to monitor fit and assess efficacy.
How do I know if a dental device for sleep apnea is working?
Follow-up monitoring, including a repeat sleep study or home sleep test while wearing the device, is typically recommended to confirm that the appliance is achieving an adequate reduction in breathing disruption events. Subjective improvements in daytime energy and reduced snoring reports from a bed partner are also common positive indicators.
Thank you for reading this article.
Latest posts
-
AI for Sleep: How Artificial Intelligence Is Changing the Way We Rest
AI for sleep has become a quiet revolution in how people fall asleep, stay asleep, and figure out what is wrong with their nights, says Dr. Avinesh Bhar, Board-Certified Sleep…
-
AI Tools to Improve Sleep Quality: A Doctor’s Guide to What Actually Helps
AI tools to improve sleep quality have moved from a niche tech trend into millions of bedrooms, says Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and many people now…
-
The Best Sleep Specialist in Indiana
Finding the best sleep specialist in Indiana takes more than a quick web search, according to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, and the right choice depends on…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.


