👉 Register for Free. How to Diagnose Sleep Apnea Faster in Primary Care – FREE Webinar by Dr. Audrey Wells. – Friday, April 24 at 12 PM ET

What to Expect During a Home Sleep Apnea Test: Step by Step
If your doctor has recommended a sleep apnea test at home and you are not sure what it involves, you are not alone. Most people who receive this recommendation have never seen the equipment, never worn the sensors, and have no idea what the night will actually feel like. The uncertainty is understandable. But the reality is far simpler than most people expect, and knowing exactly what to expect beforehand makes the whole experience significantly easier.
This guide walks you through the entire home sleep apnea test process, from the moment your kit arrives to the morning you send it back, sensor by sensor and hour by hour. No surprises.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
What is a Home Sleep Apnea Test?
A home sleep apnea test (HSAT) is a simplified sleep study conducted entirely in your own bedroom. Unlike an in-lab polysomnography, which requires spending a night in a clinical facility connected to dozens of electrodes while a technician monitors you from an adjacent room.
A home sleep test uses a compact wrist-worn device to collect the physiological data your physician needs to evaluate whether sleep-disordered breathing is present.

Home sleep tests are not appropriate for everyone. People with significant cardiac conditions, suspected central sleep apnea, or certain other health complexities may require an in-lab study instead. Your ordering physician makes that determination based on your health history before recommending a home test. For the majority of patients being evaluated for obstructive sleep-disordered breathing, however, a home sleep test is considered a clinically valid diagnostic tool by the American Academy of Sleep Medicine.
For a broader overview of the home sleep testing process and how it compares to in-lab options, the guide to home sleep apnea testing as an alternative to lab testing provides useful context.
Step One: Receiving and Checking Your Equipment
When your home sleep test kit arrives, take a few minutes to open it and review the contents before your test night.
Make sure you download the app that is required for monitoring the device. At SLIIIP we use 2 types of home sleep tests that are the Sleep Image ring and the Watch Pat. Depending on the requirements of your insurance, we will send one of these devices to your home.

Check that all components are present and that the device appears undamaged. If anything is missing or unclear, contact the provider before your test night rather than discovering an issue at bedtime. SLIIIP’s support team is available to walk you through the setup process if anything is confusing once you have the kit in hand.
Read the instruction sheet fully on the day your kit arrives, not the night of the test. Familiarity with the steps in advance means you can focus on simply following them when the time comes rather than reading and interpreting under low light at eleven o’clock at night.
Step Two: Preparing for Your Test Night
The day of your home sleep test should be as close to a normal day as possible. A few specific preparations help ensure your data is clean and useful.
Avoid alcohol and sedatives. Both alcohol and sedative medications alter sleep architecture and can suppress the natural respiratory muscle activity that the test is designed to observe. Avoiding both on the evening of your test gives your physician the most accurate representation of your typical sleep breathing patterns.
Avoid caffeine after midday. Caffeine can delay sleep onset and alter sleep architecture in ways that affect the data collected. Cutting off caffeine in the early afternoon helps ensure you fall asleep at a normal time.
Shower before bed. Clean, dry skin helps the sensors maintain consistent contact throughout the night. Oils, lotions, and residue from the day can interfere with the adhesive or electrical conductivity of certain sensors.
Sleep in your normal environment. One of the most significant advantages of a home sleep test over an in-lab study is that you are sleeping in your own bed, with your own pillow, at your usual bedtime. Lean into this advantage. Sleep in your regular sleeping clothes, in your regular position, with your regular pre-sleep routine. The more normal the night, the more representative the data.
A detailed preparation checklist is also available in the how to prepare for a home sleep study guide.
Step Three: Applying the Device
This is the step most people feel anxious about, and it is also the step that turns out to be the most straightforward. Both the WatchPAT and the Sleep Image Ring are wearable devices that require no wires, no chest belts, and no nasal tubing. Setup takes under five minutes and requires no clinical training.
If You Are Using the WatchPAT
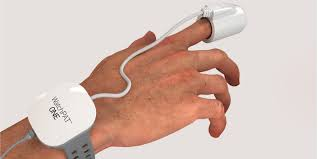
The WatchPAT consists of two components worn on your hand and wrist.
The wrist unit attaches like a watch on your non-dominant wrist. Fasten it snugly so it stays in place during sleep but not so tight that it causes discomfort. Make sure the display faces upward and the device sits flat against your inner wrist.

The finger probe attaches to your index finger on the same hand. It clips gently onto your fingertip and measures peripheral arterial tone, blood oxygen saturation, and heart rate throughout the night. The probe is lightweight and painless. Avoid applying it to a finger that has nail polish or artificial nails, as this can interfere with the optical reading.
Once both components are in place, press the start button on the wrist unit when you are in bed and ready to sleep. The device will confirm it has begun recording.
If You Are Using the Sleep Image Ring
The Sleep Image Ring is a single-piece device worn on one finger, typically the index or middle finger of your non-dominant hand. Slide the ring on so it fits comfortably with the sensor window facing the underside of your finger. It should feel secure without cutting off circulation.
SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.

The ring records continuously once worn and does not require you to press any buttons. Simply put it on before getting into bed and remove it in the morning.
A Note for Both Devices
Avoid lotions, oils, or hand creams on your fingers or wrist on the night of the test, as these can affect sensor contact. Try to sleep in your normal position. If you wake up during the night and find the device has shifted, reposition it and go back to sleep. The recording will continue uninterrupted.
Step Four: Falling Asleep
This is where most people’s concerns concentrate. Will the sensors keep me awake? Will the cannula feel strange? Will I roll over and dislodge everything?
The honest answer is that the first fifteen to thirty minutes can feel mildly unusual. You are aware of the cannula resting below your nose, the probe on your finger, and the belt around your torso. That awareness fades quickly for most people. The sensors are designed to be low-profile enough that they do not meaningfully disrupt sleep for the typical patient, and most people report falling asleep within a normal timeframe.
Rolling over during the night is completely normal and expected. The sensors are designed to accommodate normal sleep movement. The cannula has enough slack to move with you. The finger probe stays attached through typical position changes. The effort belt stretches with your torso movement. Occasional sensor displacement during the night happens in a small percentage of tests, but the recording device logs enough continuous data across the night that brief displacement periods rarely invalidate the study.
If you are a particularly light sleeper or if you know that anything unfamiliar in your sleep environment keeps you awake for extended periods, communicate this to your provider before the test. In some cases, a brief discussion about managing test anxiety beforehand is worthwhile.
Step Five: What the Device Records Through the Night
While you sleep, the recording device quietly collects data at a high sampling rate. Nothing is transmitted in real time, and no one is monitoring you remotely during the test. The device simply stores the data locally until the test is complete.
Throughout the night, it is logging your blood oxygen level continuously, tracking whether it dips below the thresholds associated with breathing disruptions. It is recording airflow through your nasal passages, noting when flow is absent or significantly reduced. It is measuring the rise and fall of your chest or abdomen, tracking breathing effort. It is monitoring your pulse rate, which rises during arousals from sleep. And in most modern devices, it is tracking your body position, noting whether you are on your back, side, or stomach, because sleep position significantly affects breathing patterns for many people.
All of this data is time-stamped throughout the night, creating a continuous physiological record that the reviewing physician uses to identify and classify breathing events, calculate your AHI, and assess the overall pattern of your sleep breathing.
Step Six: Waking Up and Removing the Sensors
When you wake in the morning, removing the sensors takes about two minutes. The nasal cannula lifts off easily. The finger probe unclips. The effort belt unbuckles. The main device is detached from wherever it was positioned. There is no cleanup beyond setting the components aside.
Some kits require you to press a stop button on the recording device when you wake. Others stop recording automatically after a set duration. Again, your instruction sheet will specify which applies.
Most kits include a pre-addressed return envelope or shipping label. The entire kit is typically returned the same day or the day after the test. Some providers use a drop-off at a local pharmacy or courier location. SLIIIP’s home sleep test kits include a prepaid return label and straightforward return instructions.
Step Seven: Results and Next Steps
After your kit is received and processed, the raw data from your recording device is reviewed and scored by a board-certified sleep physician. This review process typically takes two to five business days from the date the device is received.
The physician analyzes your overnight data, identifies and classifies each breathing event, calculates your AHI, and assesses the overall pattern. The results are then compiled into a report and shared with you, typically through the patient portal or directly from your ordering provider.
If your results indicate sleep-disordered breathing that warrants intervention, your physician will discuss the appropriate next steps with you. This may include a CPAP prescription, an oral appliance prescription, or a recommendation for further evaluation depending on the nature of the findings. If your results are within normal limits, your physician will advise accordingly, and your care team may explore other explanations for your symptoms.
To understand more about what happens after you receive results, the complete guide to getting a home sleep test covers the full process from ordering to results in practical detail. For those wondering whether their home sleep test is covered by insurance, the insurance coverage guide for home sleep studies breaks down what most major plans include.
Ready to take your home sleep test?
Order online, receive your kit at home, sleep in your own bed, and get results reviewed by a board-certified physician within days.
Common Questions About the Night Itself
What if I wake up and the cannula has come out? Replace it as best you can and go back to sleep. A brief period without the cannula seated correctly will appear as a data gap in the recording, but it will not invalidate the study as long as the majority of your sleep time is captured.
What if I cannot fall asleep? This happens occasionally and is called a first-night effect, the tendency to sleep less deeply than normal in an unfamiliar situation. Most home sleep tests are considered valid with a minimum of four hours of recorded sleep data. If you record significantly less than this, your provider may ask you to repeat the test on a subsequent night.
What if I need to get up during the night? You can get up without removing the sensors. The recording device is portable enough to move with you. Simply carry the main unit if it is detached from your wrist, and reconnect any sensors that come loose when you return to bed.
What if I sleep on my side the entire night? That is fine and actually provides useful position data. Many people with sleep-disordered breathing show significantly different AHI values depending on whether they sleep on their back versus their side. The recording device captures position throughout the night, which can inform the clinical interpretation of your results.
For those who are still unsure whether their symptoms warrant a home sleep test, reviewing the common signs of sleep apnea is a useful first step. Understanding what sleep apnea is and how it differs from simple snoring can also help you have a more informed conversation with your physician about next steps.
SLIIIP’s sleep medicine team, led by board-certified physician Dr. Avinesh Bhar, reviews all home sleep test results conducted through the platform and is available to answer questions about the process before, during, and after your test.
Is your home sleep test covered by insurance?
Many major insurance plans cover home sleep apnea tests when ordered by a licensed provider. Find out what your plan includes before you order.

SLIIIP’s board-certified sleep physicians can do sleep evaluations for sleep apnea. Virtual consultations in all 50 states. Home sleep tests shipped to your door.
Frequently Asked Questions About the Home Sleep Apnea Test
What does a home sleep apnea test measure?
A home sleep apnea test measures blood oxygen saturation, pulse rate, nasal and oral airflow, breathing effort through chest or abdominal movement, and body position. These signals allow a physician to identify and quantify breathing disruption events during sleep.
How long does a home sleep apnea test take?
The test runs for one full night of sleep. Most devices record for between six and ten hours. Setup takes approximately five to ten minutes before bed, and removal takes about two minutes upon waking.
Is a home sleep test as accurate as an in-lab sleep study?
For the specific purpose of diagnosing obstructive sleep apnea in patients without significant comorbidities, research supports home sleep testing as a clinically valid alternative to in-lab polysomnography. In-lab studies capture a broader range of data, including brain wave activity, leg movement, and detailed sleep staging, which some clinical situations require. Your physician determines which type of study is appropriate for your situation.
Can I eat and drink normally before a home sleep test?
Eating normally is fine. Avoiding alcohol and caffeine in the hours before the test is recommended, as both can affect sleep quality and breathing patterns in ways that may influence the data collected.
Will I be able to fall asleep wearing the sensors?
Most people do. There may be a brief period of adjustment when you first lie down, but the sensors are designed to be unobtrusive. The majority of patients fall asleep within a normal timeframe.
What happens if a sensor comes off during the night?
Reattach it if you notice it has come loose, and go back to sleep. A brief gap in one sensor’s data rarely invalidates the full study, provided enough continuous recording time is captured across the night.
Can I go to the bathroom during the night?
Yes. You can move around normally during the night. The recording device is designed to be portable, and sensors are fitted to accommodate natural movement.
Do I need to stay awake until a certain time before starting the test?
No. Start the test when you would normally go to sleep. A typical night’s sleep provides more than enough recording time. Staying up late to increase recording duration is not necessary.
What is the minimum amount of sleep needed for a valid home sleep test?
Most providers consider a minimum of four hours of recorded sleep data sufficient for a valid study. If significantly less than this is recorded, your physician may request a repeat test.
How long does it take to get home sleep test results?
Results are typically available within two to five business days of the device being received by the processing facility. SLIIIP aims to return results as quickly as possible following receipt of the device.
Does a home sleep test show sleep stages?
Standard home sleep tests do not capture the electroencephalogram (EEG) data needed to score precise sleep stages in the same way as an in-lab study. They record the physiological signals most relevant to identifying and characterizing obstructive sleep apnea.
What AHI score on a home sleep test indicates sleep apnea?
Most clinical guidelines use an AHI of 5 or more events per hour as the threshold for a positive sleep apnea finding. Severity classifications increase from mild (5 to 14) through moderate (15 to 29) to severe (30 or more). Your reviewing physician interprets your specific results in the context of your overall clinical picture.
Can a home sleep test detect central sleep apnea?
Some home sleep test devices can flag patterns consistent with central apnea events. However, the definitive diagnosis of central sleep apnea or complex sleep apnea typically requires the more detailed data captured by an in-lab study. If central apnea is suspected, your physician will advise on the appropriate diagnostic approach.
Do I need to sleep on my back for the test?
No. Sleep in your normal position. The device records your body position throughout the night, which is itself a useful data point. Many people show position-dependent breathing patterns that inform the clinical interpretation of results.
What should I do the morning after the test?
Remove the sensors, power off the device if instructed to do so, and return the kit using the prepaid label or return instructions provided with your kit. Contact your provider if you experienced any difficulties during the night that may have affected the recording.
Is a home sleep test painful or uncomfortable?
No. The sensors are non-invasive and designed to be worn during sleep. The nasal cannula, finger probe, and effort belt are all lightweight and do not cause pain. Initial awareness of the sensors is common but typically fades within the first half hour.
Can children take a home sleep apnea test?
Home sleep testing for children is less standardized than for adults, and many providers recommend in-lab polysomnography for pediatric patients. Your child’s physician will advise on the most appropriate evaluation approach based on age and symptom profile.
What if my home sleep test results are negative but I still feel unwell?
A negative home sleep test result rules out obstructive sleep apnea as a cause of your symptoms but does not rule out other explanations for poor sleep quality or daytime fatigue. Your physician will discuss alternative possibilities and next steps based on your full clinical picture.
Is a prescription required to order a home sleep test?
A physician order is typically required. Through SLIIIP, the ordering process is handled entirely online. A brief intake questionnaire is reviewed by a physician who determines whether a home sleep test is appropriate before the kit is dispatched.
How do I get a home sleep test through SLIIIP?
You can order a home sleep test directly through the SLIIIP home sleep test page. The kit is delivered to your home, you complete the test in your own bed, and results are reviewed by a board-certified sleep physician within a few business days of the device being returned.
Thank you for reading this article.
Latest posts
-
Best Treatments for Insomnia Caused by Anxiety
The best treatments for insomnia caused by anxiety hit both sides of the loop at once, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, has watched this two-front approach…
-
Best Nighttime Routines for Mental Health
The best nighttime routines for mental health do more than just help with sleep, and Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, has watched the right evening habits steady…
-
Can Sleep Apnea Cause Anxiety or Depression?
Sleep apnea, anxiety, and depression can blur into one tangled mess until the right evaluation pulls them apart, and according to Dr. Avinesh Bhar, Board-Certified Sleep Physician at SLIIIP.com, the…
Get updates
Spam-free subscription, we guarantee. This is just a friendly ping when new content is out.


